
As the first members of Canada’s baby boom generation turn 65, the official age of retirement, this study by gerontologist Neena Chappell provides a timely overview of the main health and social policy challenges presented by population aging in three areas: informal care, formal care, and prevention.
There is much argument and debate among experts as to whether Canada’s existing public programs will be sustainable with the increases in the number of seniors and their higherthan-average use of health and social services. However, it is factors other than population aging, such as increased medical interventions, changes in expensive technologies and increases in overall service utilization, that are mainly driving costs in the health care system. While present and upcoming demographic challenges do not warrant alarmist reactions, governments need to plan well ahead to ensure there is appropriate and effective care for an aging Canadian society.
Chappell first looks at the evolving care needs, and shows that in the coming years, more seniors will depend on fewer individuals to provide the care they need. While it is true that elderly people are likely to suffer from chronic conditions, not every chronic condition will translate into a disability. It remains unclear whether baby boomers will have better or worse health or will live longer than those who are currently elderly, as the incidence of some diseases is declining while that of others is on the rise.
The author underscores that when health fails, however, support by unpaid family and friends is the mainstay of care. Women are more likely than men to be caregivers, and the caregivers might themselves be seniors. Caregivers commonly experience stress and burden, especially when caring for people with dementia. Currently the health care system acts as a safety valve when family care is unavailable or insufficient, and the only public support for informal caregivers is the provision of short-term respite to ensure the continuity of family care.
Developing policies that support the needs of informal caregivers is important. In addition, there is a need for formal long-term home care as lower fertility rates, increasing rates of divorce, remarriage and blended families may affect the provision of care by family members. The assumption that medical care is the most appropriate means to ensure the health of an aging population needs to be re-examined.
We need to establish a comprehensive home care system that links and partners with informal caregivers and community organizations to form a support network for informal caregivers and care recipients; one that is also integrated into the overall health care system. This would be cost-effective and is the most appropriate option for an aging society.
In 2011 the first members of Canada’s baby boom generation turned 65, drawing attention to the demographic trends gerontologists have been discussing for years. Because physical health declines with the aging process, which is characterized by chronic conditions for which there is no cure, the prospect of cohorts of baby boomers reaching their 70s and then their 80s raises concerns about the provision of care. Moreover, the baby boom generation is, at present, providing most of the necessary care to those who are already elderly. That is, their significance extends beyond the fact that they will constitute a large cohort of older adults in the near future and includes their caregiving role at the present time.
Although the aging of Canadian society does not warrant alarmist reactions, we need to plan realistically for current and upcoming demographic challenges. We can draw upon more than 35 years of gerontological research here and abroad about appropriate and effective care for an aging society.
Indeed, the problems in this area are well known and have been for some time. A decade ago, the Canadian Association of Retired Persons (now the Association of Fifty-Plus) listed the following challenges as requiring immediate attention: lack of leadership and of a coherent strategy for developing home care, shortage of human resources, inadequate funding, caregiver burden, pressures on the voluntary sector, diminished and inequitable access to home care, medicalization of home care, increased privatization, reduction in home support, variation in service, lack of knowledge and awareness, and lack of research (Canadian Healthcare Association 2009). Except for the last two, these issues remain unaddressed. Governments to date have not embraced aging as a fundamental framework for defining social policy.
This paper draws on what we know in order to provide broad guidelines for public policy. The paper focuses on care, both informal and formal, and on the role of public policy in the provision of that care. I first examine care needs among older adults and then discuss policy challenges and options. In short, I argue that the challenge is to establish a comprehensive community care system to ensure that necessary health and support services are provided based on needs, to recognize informal caregivers in the process and to do so within an integrated care system.
Concerns have been expressed over the rising tide of older adults in Canadian society. “Apocalyptic demography” is the oversimplified belief that a demographic trend such as population aging inevitably has dire consequences. For instance, it is often assumed that because of the impending growth in the number of seniors and their higher-than-average use of health and social services, the country cannot sustain these public programs (Gee and Gutman 2000). This is an overly alarmist view of our aging society.
The overall dependency ratio (including both those over age 65 and those under age 15, as a ratio of persons of working age, aged 15-64) was at a historic low in 2006 at 44, down from 2001 at 62 (meaning there were 62 older and younger people for every 100 working-age persons). It is projected to be only 61 in 2031 and 69 in 2056. However, Statistics Canada revealed a rise in the proportion of persons over age 65 from 11.5 percent of the total population in 1991 to 12.5 percent in 2000 and 13 percent in 2006 (Alberta 2008, 2009; Statistics Canada 2008a); projections indicate a further rise to between 23 percent and 25 percent in 2036 and between 24 percent and 28 percent in 2061. In addition, the old age dependency ratio (those over age 65 as a ratio of those of working age, aged 15-64) does show a steady increase, causing concerns that society cannot afford the care of persons over age 65: 16.6 in 1991, 18.3 in 2000 and 20 in 2006, and it is expected to reach 39 in 2036 (Statistics Canada 2009a).
The true rate is probably higher. Revisions to the estimates of the overall and old age dependency ratios now define the youth population as those aged 0-19 (it was 0-14 before) and the working-age population as those aged 20-64 (15-64 before), thus increasing the size of the youth population and shrinking the size of the working-age population. This results in an increase in the overall and old age dependency ratios. Using these definitions, between 1971 and 2006, the overall dependency ratio decreased from 89 to 60, and it is projected to increase to 84 by 2056. The old age dependency ratio increased from 15 in 1971 to 21 in 2006 and is projected to be 40 by 2056 (see figure 1). Given changes in educational patterns, which see youth pursuing schooling for longer periods of time, this is probably a more accurate reflection of current trends. However, if the disappearance of mandatory retirement results in an increase to the normal retirement age and, therefore, in the size of the working-age population and a decrease in the size of the old age population, a further adjustment of the formulas used to compute dependency ratios will likely reduce the size of the old age dependency ratio, so the current figure will not then be accurate.
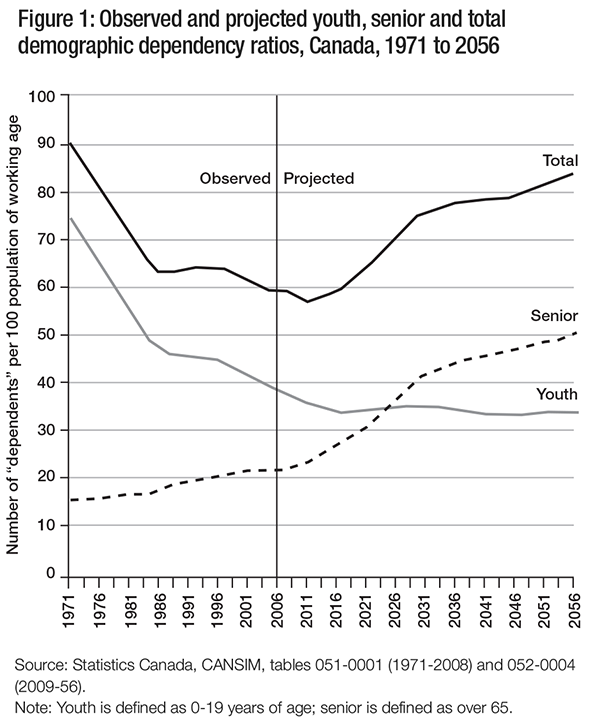
Whether an increase in the old age dependency ratio entails increasing and perhaps unaffordable health care costs is a matter for debate. The future escalation in health care costs per se is not the question addressed here. Rather, the focus here is the extent to which rising costs are attributable to the increasing number and proportion of older adults.
Economists Magnus (2009) and Robson (2009) argue that the cost of care for children is less than the cost of care for older adults, and that the decline in the proportion of young people will not offset the greater cost of caring for older adults; thus the potential cost of caring for older adults could be unaffordable. Similarly, Robson (2001) estimates that the implicit health care services liability associated with the pressure of an aging population amounts to more than 50 percent of Canada’s gross domestic product (GDP).
However, whether these costs can be contained while providing adequate care for older adults depends on what their needs are. Mendelson and Divinsky (2002) argue that while those age 75 and over make disproportionate use of health care services, that age group will grow only from 5.8 percent of the population in 2001 to 6.7 percent in 2016. Even if it is assumed that they consume 50 percent of all health care expenditures, their growth will likely add only 1.1 percent to health care expenditures as a percent of GDP. This number, while not insignificant, is well under expected economic growth. “In other words, everything else being equal, health care expenditures would increase to 10.1 percent of GDP by 2016 due to the increased number of elderly. This represents a real cost pressure, but it is hardly the Armageddon of health costs” (35, n5).1
Similarly, economists Denton, Feaver and Spencer (1998) and Denton and Spencer (1999) argue that Canada can easily afford an aging population, given at least moderate levels of economic growth. The Health Council of Canada (2008) notes:
Contrary to popular belief, aging and population growth are not the major causes of the rises in Canada’s health care spending. The largest factor is our increase in use of services. On average we are all getting more care, undergoing more tests, and receiving more prescriptions. Are we healthier as a result? If we aren’t, are we prepared to continue to pay more anyway?…The persistent belief that our aging population will overwhelm the health care system is a myth.
In addition, research in Manitoba (CHSRF 2001) has established that most of the older adults using more services are healthy seniors, which means that healthy, not sick, adults are driving most of the increased usage (accounting for 57.5 percent of the increase in the late 1990s). Furthermore, the rising costs of technological interventions (including pharmaceuticals) are a major factor in medical cost increases, much larger than the aging of the population (Di Matteo 2005). Finally, Morgan and Cunningham (2011) find that per capita expenditures on acute hospital care and doctor visits increased only slightly more than inflation (17 percent) between 1996 and 2006, while spending on prescription drugs increased by 140 percent. Thus, increased medical intervention and changes in patterns of health care practices account for the rising costs, yet we lack the evidence that they are appropriate and necessary or that they increase the health and quality of life of older adults (Barer, Evans and Hertzman 1995).
There is much argument and debate in this area. At minimum, there is evidence indicating that while society should take the increasing numbers and proportions of older adults seriously, other factors are much more important than the changing demographics in the extent and affordability of health care costs.
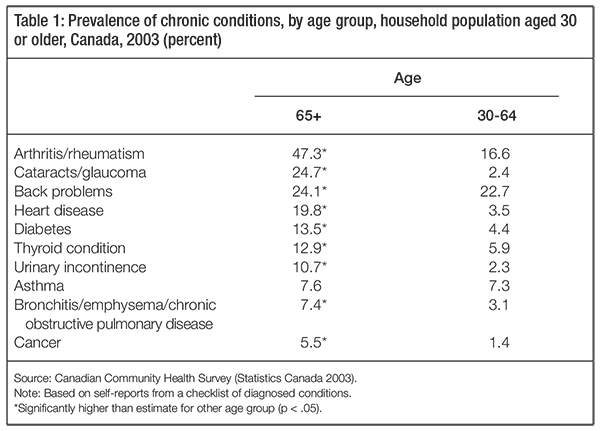
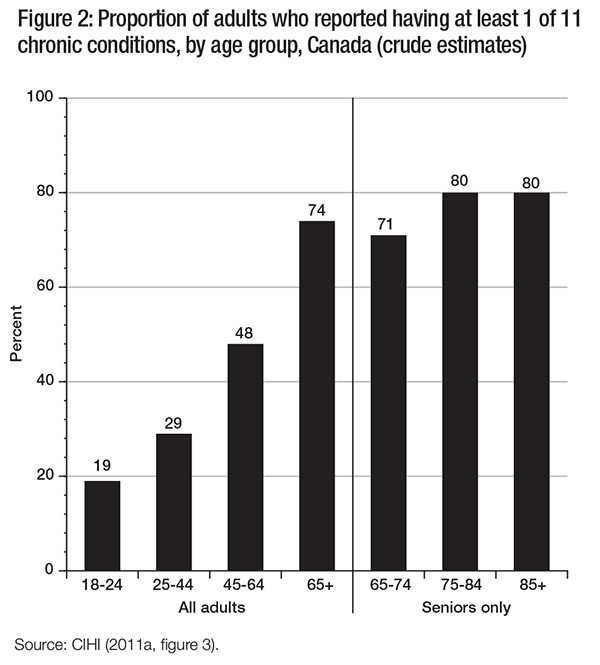
What are our care needs in old age? As we age, physical health declines and the prevalence of chronic conditions increases (see table 1). Common chronic conditions include arthritis, diabetes, heart disease, high blood pressure and mood disorders, not including depression (CIHI 2009). Most of those over age 65 have at least one chronic condition (see figure 2). The prevalence is higher among women than men, especially for arthritis/rheumatism, cataracts/glaucoma and back problems, although men are more likely to have heart disease, diabetes, cancer and Alzheimer’s disease (DesMeules, Turner and Cho 2004; Gilmour and Park 2006). Living with chronic pain is also relatively common, with 27 percent of seniors reporting chronic pain; 16.7 percent of men and 23.9 percent of women over age 65 suffer from pain that prevents activities, higher proportions than in any other age group (Statistics Canada 2008b, 2010a).
However, suffering from a chronic condition does not necessarily translate into incapacity — that is, into a limitation on one’s functioning (Partridge, Johnston and Morris 1996). While 81 percent of those over age 65 suffer from at least one chronic condition, fully 80 percent of them are functionally able to live independently.2 Nevertheless, activity restriction does increase with age: 12 percent of those aged 15-64 but 43 percent of those aged 65 and over experience some restrictions (56 percent of those aged 75 and over) (Statistics Canada 2007). Women are more likely to experience activity restriction than are men (DesMeules, Turner and Cho 2004).
Disability is usually defined in terms of restrictions in one’s ability to perform activities of daily living or to function independently in terms of basic activities of daily living or instrumental activities of daily living (Heikkinen 2003). Mobility disability is particularly serious because being able to ambulate is critical to so many other activities that allow us to remain independent. There is wide recognition that disability refers to a relational perspective beyond simply diagnosing physical ability; it includes complex relationships between an individual’s health condition and personal and external factors in the environment (WHO 2001). The term “disablement process” refers to a dynamic interaction interwoven with cultural norms and socio-economic status, encompassing attitudes, emotions, stigma, accessibility or lack thereof of various services, wheelchair-accessible buildings and so on.
It is to be noted that women experience more disability than men, and while severe disability is related to higher rates of mortality among both men and women, women nevertheless survive longer and with more disability (Chappell and Cooke 2010). The old elderly are also much more likely to experience disability than are the young elderly — for that reason the World Health Organization (WHO) argues that, in terms of disability, old age can be viewed as starting at age 75. While recent reports of declining rates of severe disability in some countries have led to optimism for the future, the trend does not characterize all nations and does not characterize Canada, where the trend is currently stable (OECD 2009; Manton 2008).
The major mental disease of concern in old age, dementia — of which Alzheimer’s is the most common type — also increases in older age. The Canadian Study of Health and Aging (1994), Canada’s first and only national study establishing the prevalence of dementia, documented that between 7 percent and 8 percent of older adults over age 65 have this disease, with women more likely to have dementia than men, which may change if men reach women’s life expectancy (Hill et al. 1997). Less severe symptoms of mild cognitive impairment are experienced by another 16 percent of older adults (National Advisory Council on Aging 2004).
Whether baby boomers will have improved or worse health in older age than those currently elderly is unclear. Wister (2005) reports that rates of cardiovascular disease, arthritis/rheumatism, hypertension and bronchitis/emphysema have been declining from the 1970s to the late 1990s. However, rates for diabetes, migraine headaches, and asthma and other respiratory diseases, as well as the total number of chronic conditions, have increased in the same time period. Current concerns over increasing rates of obesity raise the possibility that the current generation of young adults might not live longer than, or even as long as, their parents and that current trends toward the compression of morbidity might not continue much into the future. Russia’s recent drop in life expectancy (Magnus 2009) dramatically demonstrates the real consequences of poor health.
Canadian seniors perceive themselves as having poorer health, compared with the self-perceptions of younger adults: only 39.3 percent of men and 38.9 percent of women over age 65 report their health as excellent or very good, the lowest proportions of all age groups (the figures are 48.8 percent and 53.2 percent respectively for those aged 55-64, the next-lowest figures). A decline with age is also found in perceptions of mental health, although the figures are considerably higher than for physical health and the gap with younger age groups much less important; 70.1 percent of elderly men and 69.4 percent of elderly women say their mental health is excellent or very good (the figures are 72.7 percent and 73.3 percent respectively for the next-lowest age group, those aged 55-64) (Statistics Canada 2010a,b).
Thus, objective and subjective measures show that health declines as we age and continues to decline during older age. Interestingly, however, these health difficulties do not necessarily translate into lessened psychological/emotional health or subjective well-being. The reason for this is not known. It is speculated that in old age, many of the concerns of younger adulthood such as having a job and raising a family are no longer as salient and/or that older adults compare their situation with that of others who are worse off (such as those who have passed away).
Statistics Canada (2007) reports that seniors, particularly those aged 65-74, experience more life satisfaction than adults aged 25-64. In addition, depression rates decrease with age. In 2002, only 1.9 percent of women and 2.1 percent of men over age 65 suffered from depression in the previous 12 months, compared with 5.6 percent and 3.5 percent respectively for those aged 4565 (the next-lowest age group). Those aged 15-24 are the most likely to suffer depression (8.3 percent of women and 4.5 percent of men). Until age 65, women are more likely to be depressed, but afterwards they are less likely to experience depression than are men (Canada 2006). There is some concern, however, that depression is underdiagnosed among seniors.3
Similarly, levels of happiness decrease after age 24, reaching a low among 35-44-year-olds, and then increase until those aged 55-64 are as happy as those aged 18-24; those over age 65 are much happier (Helliwell 2003). In 2010, a large majority of women aged 65 and over (92.6 percent) and the same proportion of men said they were satisfied or very satisfied (Statistics Canada 2011).
Still, there are increasing health difficulties during old age with which individuals must cope and for which they frequently require care. This is especially true for those who become frail. Even though frailty does not characterize everyone in old age, the term does apply to a substantial proportion of seniors, and the proportion increases as the population ages.4 Frailty is broader than disability alone and includes dependency; it is a vulnerability resulting from the interaction of the simultaneous deterioration in many organ systems leading to adverse outcomes but without reference to a particular disease itself. Hogan, MacKnight and Bergman (2003) note an emerging consensus that frailty largely refers to a state of vulnerability to experiencing adverse outcomes. Rockwood and Mitnitski (2007) refer to it as “a nonspecific state of increasing risk, which reflects multisystem physiological change” (722).
Care needs are not evenly distributed. They are higher among certain subpopulations. Poverty is a risk factor for many adverse health experiences (Huguet, Kaplan and Feeny 2008; Kaplan et al. 2010; McIntosh et al. 2009), and even though the percentage of older adults living in poverty has been declining, poverty in old age has not disappeared; many live just above lowincome thresholds. The proportion of seniors with incomes below the low-income cut-off fell from 37 percent in the early 1970s to 5.9 percent in 2004 (National Seniors Council 2009). However, unattached individuals are more subject to living in poverty compared with couples, and relatively more women live in poverty than men:
The unattached have the highest incidence of low income of any group, with 15.5 percent of unattached seniors living below LICO [low income cutoff], a rate 11 times higher than that of senior couples (1.4 percent). Given their greater longevity, women are far more likely to be unattached in later life and at greater risk of experiencing low income. Indeed, women represented about three-quarters of the 179,000 unattached low-income seniors in 2006. The low-income rate for unattached senior men was 14.0 percent, compared to 16.1 percent for unattached senior women. (National Seniors Council 2009)
That is, those who are poor, female and unattached are more likely to require care and assistance in old age than are those who have more economic resources, are male and are attached.
Social isolation is another risk factor during old age, although it is not a problem for most. While most older adults in modern Canadian society are retired and are thus outside of mainstream economic society, they are, by and large, socially embedded, especially within families. The notion of a modified extended family, as described more than four decades ago by Eugene Litwak (1960) — emphasizing mutual close intergenerational ties among kin, strength of intergenerational relations, continuity of responsible filial behaviour and contact between the generations — is a more accurate description of most older adults’ social interactions than isolation.
In 2003, 98 percent of Canadian older adults said they had a family member or a friend they felt close to (Lindsay 2008; Statistics Canada 2009b). Most also have companionship and confidants (Chappell, MacDonald and Stones 2008; Cranswick 2003), and interaction between older Canadians and their adult children is characterized by intimacy-at-a-distance, a term coined by Rosenmayr and Kockeis (1963) half a century ago. It describes older adults’ general preference not to live with their children but to maintain close ties. When asked only about friends, 12 percent to 14 percent of those aged 65-74 say they have none, compared with 5 percent of those aged 25-54. The figure is 18 percent for those aged 75 and over (Lindsay 2008; Statistics Canada 2009b). That is, most older adults are not socially isolated, but for those who are, it can be a risk factor for poor health and requiring care.
In addition, there remain ageist attitudes throughout society. Ageism is the treatment of older people as a social category. Such attitudes have been documented, for example, in media portrayals of seniors, among school-aged children, among health care professionals and among employers facing older job applicants (Achenbaum 1995; Van Dalen, Henkens and Schippers 2009; Wood, Wilkinson and Harcourt 2008). In fact, the low level of interest of individuals in occupations related to older age (Gonçalves 2009) is of such concern that several national organizations in Canada, including the Association of Geriatric Physicians and the Canadian Association on Gerontology, formed a group known as the Geriatric Education and Recruitment Initiative, whose task it is to change the negative image of older adults within society (Hogan 2007). The pervasiveness of ageism has led Stones and Stones (1998) to refer to it as a “quiet epidemic” that contributes to indifference. Interestingly, ageism does not necessarily lead to interpersonal antagonism: we may treat our grandmothers well but simultaneously refer to and treat other older adults with indifference and even contempt.
In sum, there is much we know about seniors’ health. Our health declines and continues to do so in older age. The extent and type of decline vary considerably from individual to individual, and while not everyone is characterized by incapacitating ill health, many experience different forms of decline, and those most at risk of serious problems can be identified. The most vulnerable are the old elderly, the poor, and those who are socially isolated and living alone.
Given the needs of an aging society and Canada’s existing health care system, what policy challenges lie ahead? The next sections examine some of the challenges and possibilities for meeting them in three general areas: informal care, formal care and prevention.
The issue of who provides care for older adults is a question of the boundaries between state and family: that is, who should be providing what care and how much.
When health fails, support by unpaid family and friends, notably family, is the mainstay of care in old age even though, in modern Western society, an individualist and not a collectivist ideology prevails, one that does not explicitly teach norms of adult children caring for their aging parents. This contrasts with the view of old age in some other cultures, particularly collectivist cultures. Asia stands as an example where there is reverence for seniors and explicit teaching of the notion of filial piety: care and respect for one’s parents as they age (Chappell 2007). Despite differing societal norms, families everywhere, including in the West, also care for their aging members and have always done so. Unpaid care for family and friends is the mainstay of care to older adults. Even with women entering the paid labour force and changes in family forms, families still provide care. Lafrenière and colleagues (2003) and Cranswick (2003) report that 70 percent of the hours provided for housework, shopping, meal preparation and personal care — the four activities most related to long-term home support — are provided by members of the informal network and that 39 percent of elderly women and 46 percent of elderly men receive all of their care from informal sources (representing no change from 1996).
Caregiving is support provided to individuals when their health has deteriorated and they can no longer function independently (Chappell, MacDonald and Stones 2008; Chappell and Funk, forthcoming). Diverse terms are found in the literature and are often used interchangeably, without definition, and without definitional consensus, including caregiving, caring, assistance, interaction, support, informal caregiving, family caregiving and others. Informal care is the major form of care in old age, far exceeding that provided by the formal health care system (Chappell, MacDonald and Stones 2008). In 1990, Kane concluded, after examining research across industrialized countries, that the informal network provided 75 percent to 85 percent of the total personal care received by seniors, irrespective of whether the country provided comprehensive health insurance (Kane 1990). Research since that time has not indicated a significant change. At any one time, most older adults receiving care do so for instrumental activities of daily living, such as shopping and transportation, and not basic activities of daily living — that is, those activities required for survival, such as eating and toileting.
Many studies have estimated caregiver contributions either at minimum wage or in terms of replacement value, demonstrating the care and nurturing that is provided in these relationships (Harrow et al. 2004; Langa, Fultz et al. 2002; Langa, Vijan et al. 2002). A recent Canadian study (Hollander et al. 2009) documents involvement in meal preparation and cleanup, housecleaning, laundry and sewing, maintenance and outdoor work, shopping for groceries and other necessities, providing transportation, doing banking and bill paying, and personal care (assistance with bathing, toileting, care of toenails and fingernails, brushing teeth, shampooing and hairdressing). A conservative estimate from that study is that informal caregivers, aged 45 and over, provide approximately $25 billion of care yearly to older adults in Canada. The authors note that providing care is something that caregivers typically want to do and prefer to do rather than having formal care come into the home. They do not suggest that all informal care be replaced with formal care, but rather that caregivers should be supported in the care they willingly provide.
Women are more likely to be caregivers than are men, and spouses are the first resort for care. Women, who have longer life expectancy and who often marry men older than themselves, tend to be there to provide care as their husbands’ health declines; once a woman is widowed, typically a daughter steps in to provide care for her mother. Women are also more likely to provide more care in terms of total weekly hours and in terms of homemaking, personal care, emotional support and the organization of care. Men are more likely to provide instrumental assistance with things such as home repair (Chappell and Kusch 2007; Keating et al. 1999). It is to be noted, however, that when there is no female available, sons do step in and provide the care.
Women predominate as caregivers because of both social structure and ideology. Social structure, reflected in government, employment organizations, health insurance arrangements and so on, limits the formal assistance that is available, which in turn necessitates informal assistance. In addition, ideologically, paid work has been the primary forte of men whereas caregiving has been part of women’s nurturing role (Walker et al. 1998). The mating gradient, established when women marry or cohabit at younger ages than men, facilitates these gender differences. The term refers to a widening, over time, of the initial differential between the wife’s and the husband’s economic resources. Men are often involved as support to a sister or a wife who is the primary caregiver to an aging parent.
It is important to remember that caregivers can themselves be seniors. Cranswick (2003) and Stobert and Cranswick (2004) report that a quarter of caregivers are seniors providing care to other seniors. This includes both spouses and older children, who are now themselves elderly, as well as friends and neighbours.
Much of the caregiving research has been dominated by a practical or social problems orientation (Dannefer et al. 2008). While there is a literature that distinguishes emotional aspects of caregiving (caring about the person and emotion work), these aspects continue to receive less attention than the tasks of caregiving (such as assistance with basic and instrumental activities of daily living); nevertheless, it is the emotional aspect that, along with the presence or absence of remuneration, by and large distinguishes informal from formal caregiving (Calasanti and Slevin 2001; MacRae 1998; Wenger, Grant and Nolan 1996), though things seem to be changing. Distinctions between informal and formal care are blurring as family caregivers undertake more skilled tasks traditionally performed by professionals (Ward-Griffin and Marshall 2003), while formal care providers describe emotional, even family-like relationships with their clients (Chappell 2008; Lan 2002). These distinctions are becoming even more complex as some elderly persons pay informal caregivers either directly or indirectly or receive formally organized volunteer (i.e., not paid) support.
There is also an increasing recognition that those providing care and assistance to older adults may not necessarily define themselves as caregivers, nor see what they do as “work” (Henderson and Forbat 2002; O’Connor 2007). And the point at which support evolves into caregiving per se is not well understood. Boundaries between caregiving and normal or everyday assistance, if individuals are capable of undertaking tasks themselves but assistance is provided within reciprocal exchanges or interdependencies, is also understudied (Henderson and Forbat 2002; Martin-Matthews 2000).
A major focus within the caregiving literature in gerontology is on the stress and burden experienced by adult children providing care to their parents, especially those caring for persons with dementia. “Hidden victims,” “sandwich generation” and “generation in the middle” have become popular terms in the media. These terms, however, are misnomers; “serial caregiving” would be more accurate. Penning (1998) and Williams (2005) have documented that no more than a quarter of middle-aged caregivers are caring for children at home and for a parent at the same time. Typically, care of a parent takes place after children have grown and left the home (Chappell, MacDonald and Stones 2008). Most women raise their children, then care for their parents, and then care for their husbands, in succession.
The stresses of caregiving are also well documented; they include depression, guilt, worry, anxiety and loneliness, emotional stress and strain, lower physical functioning, lower social functioning, and worse general health (Canuscio et al. 2002; Hirst 2005; Ho et al. 2009; Ory et al. 1999; Christakis and Allison 2006). Vitaliano, Zhang and Scanlan (2003) conducted a metaanalysis of 23 studies of negative health impacts for family members caring for older persons and concluded that caregivers are at a higher risk of negative physical health outcomes than non-caregivers. Among caregivers, those who are at greater risk are those who are experiencing strain (Schulz and Beach 1999), experiencing difficulty (Navaie-Waliser et al. 2002), feeling overburdened (Sherwood et al. 2005), providing more extensive assistance (Pinquart and Sörensen 2003) or providing care to seniors who have particularly severe mental and/or physical impairment and dementia-related behavioural problems (Pinquart and Sörensen 2003, 2007). Caregivers with low income (Bakas and Burgener 2002; Robison et al. 2009), those with lower formal educational levels (Navaie-Waliser et al. 2002), older caregivers (Navaie-Waliser et al. 2002) and females (Canuscio et al. 2002; Ho et al. 2009) are also at greater risk.
There is so much attention paid to the negative consequences of caregiving that it is easy to assume there are no satisfactions from this role. However, research demonstrates that the majority of caregivers are able to cope, and they do not feel overly burdened, or if they do, it is periodic, not constant (Chappell and Dujela 2008). Furthermore, caregivers experience selfaffirmation, enjoyment and a sense of satisfaction (Braithwaite 1998; Tarlow et al. 2004). Interestingly, less than 5 percent of caregivers to older adults indicate that they are not doing well (Statistics Canada 2008a,b). At the same time, 70 percent report that providing care has been stressful. This is true even among those saying that they are coping very well; 70 percent also say they need a break, either frequently or occasionally (Health Canada 2002).
Thus, while caregiver burden is related to overall well-being, it is a separate concept, such that caregivers can be burdened in that role while nevertheless experiencing good overall wellbeing (Chappell and Reid 2002). Furthermore, caregivers can experience both negative and positive aspects of the role simultaneously (Andren and Elhmstahl 2005). The extent to which the expressions of the positive aspects of caregiving reflect social desirability and/or caregivers’ attempts to cope with the difficulties of caregiving by focusing on the positive is not known (Funk and Stadjuhar 2009).
As noted by Keefe and Rajnovich (2007), virtually all countries accept the notion that families have some responsibility to care for their members. And research tends to show that providing care is something that informal caregivers typically want and prefer to do rather than having formal care providers come into the home. This suggests that one of the first policy interventions required is to support caregivers in the care they willingly provide. But at the present time, except for a few modest tax measures or programs (such as the compassionate care leave available through the employment insurance program), there is no national policy addressing family members (or others) caring for disabled older adults in Canada. Home care programs are under provincial jurisdiction.
British researcher Linda Pickard (2001) notes two basic approaches to government policy on caregivers. One is to support the continuation of family care through the provision of shortterm breaks to caregivers with the aim of assisting them in the continuation of this role. The other, the “carer blind” approach, uses an assessment of seniors’ needs that does not take the existence or capabilities of a caregiver into account in deciding service eligibility. In this approach, formal services could substitute for informal caregiving, arguably giving the care receiver greater autonomy and the caregiver greater freedom.
In Canada, only the first approach is used. It is assumed that a large amount of family care is available; family caregivers do not benefit from any direct public support. The health care system acts as a safety valve when family care is not available or not sufficient. And, at the point of entry into the health care system, policy typically is oriented toward the older adult, not the needs of caregivers or the caregiving unit. That is not to say that caregivers are ignored in the decisions as to what and how much formal care is provided, but policy does not usually involve joint decision-making with one of the decision-makers being the family caregiver.
Typically the only service that is targeted to caregivers is respite care, appearing in three guises: sitter attendance services giving short breaks to the caregiver to run errands, go to a doctor’s appointment and so on; adult daycare, where the older adult leaves the home for a few hours a week; and respite care beds within nursing homes for short stays. At the present time, there are no other programs that target caregivers, and in some jurisdictions (for example, British Columbia), caregivers are eligible for respite services only when the older adult is already receiving formal care services. Those who are doing such a good job that the recipient does not need formal services are, by definition, not considered for support.
This is not to say that services delivered to the older adult are unimportant in supporting the caregiver. Services provided to the older adult can allow respite, needed rejuvenation and rest for the caregiver and can help prolong the caregiver’s involvement, an option that most caregivers state they prefer; but this requires caregivers’ needs to be taken into account (Chappell, Reid and Dow 2001; Hollander et al. 2007). Surprisingly little research attention is paid to the relationship between family care and the receipt of formal care, one that has been shown to be complementary, rather than one of substitution; formal care is called upon either when there is no informal care or when the demand is such that informal caregivers cannot cope on their own (Chappell and Blandford 1991; Dossman, Fast and Keating 2005).
Policies that support the needs of caregivers are important for several reasons: the formal care system could never replace all of the support provided informally; caregivers express a desire to continue in this role; and many caregivers make great sacrifices in order to provide the care that they do. Without assistance, caregivers’ health can deteriorate and result in greater demands on the formal health care system at a much greater cost. Such policies are particularly important for women, who constitute the majority of caregivers. However, policies may inadvertently encourage women to leave the labour force, thus pushing them back into the private sphere and reinforcing the gendered division of labour. If women are quitting work and reducing employment to provide care anyway, support may provide real assistance and recognition of the value of their contributions. If we believe individuals should have choices, support for caregivers must be sufficient so the individual has alternatives, in terms of both whether to be a caregiver and the extent of caregiving provided. Keefe and Rajnovich (2007) summarize the issue:
The debate should focus less on whether family or state should be responsible for providing care, and focus more on how caregivers can be supported if they choose to be a caregiver, while ensuring that the choice does not carry [negative] shortand long-term consequences. Policy must be based on the needs of persons of all ages in the society, not just those in need of care. It must also consider the interconnections among individuals and families and how social policy affects these relationships. (87)
In 2008, the Canadian Caregiver Coalition suggested that the value of family caregiving should be acknowledged in legislation, policy and practice, and proposed a framework that has these essential elements: to safeguard the health and well-being of family caregivers and increase flexible and available respite care; to minimize excessive burden; to enable access to user-friendly information and education; to create work environments that are flexible and respect caregiving obligations; and to invest in research and evidence-informed decision-making in this area. Such a guiding framework can provide a yardstick or benchmark against which progress or the lack thereof can be assessed.
It might also be noted that support for the caregiver can and often does take the form of arrangements outside of the formal health care system, including voluntary organizations, churches and other not-for-profit and neighbourhood organizations as well as informal groupings of friends and neighbours. The health care system at present is not organized to act as a coordinator or broker for bringing any such resources together. There is no place in society mandated with this task. Some targeted experiments, however, suggest this is achievable. For example, the McConnell Foundation of Montreal gave funds to various groups within the formal care system with a mandate to not do business as usual. They were tasked with providing respite to caregivers in need in rural areas on an innovative basis, in which caregivers themselves defined what would give them a break. Drawing on the concept of respite as an “outcome not a service” (Chappell, Reid and Dow 2001), the program devised solutions for each client that responded to individual needs while taking into account the caregivers’ context of family, friends, neighbours, volunteers, and health care and social services, coordinating and drawing on any number of these sectors.
An examination of three such rural projects (Chappell, MacDonald and Stones 2008) concluded there were six foundational principles for facilitating such respite: embracing caregivers as partners; raising awareness of caregiving issues among caregivers themselves, their family and friends, and the general public; networking and engaging stakeholders; creating advisory structures inclusive of the key stakeholders; caregiver leadership; and building community capacity that encourages creativity and individualizing support.
In addition to providing direct services to caregivers and adequate labour policy (including labour standards and employment insurance), the Special Senate Committee on Aging (2009) recommended providing direct payment to caregivers for reimbursement of expenses, and compensation and indirect financial support such as tax credits, pension credits and dropouts from pensions. The committee also recommended that the federal government play a lead role and that all levels of government work together to ensure that caregiver needs are formally recognized and integrated into policy and delivery of formal health care services (Hollander et al. 2007).
While family caregiving is the dominant form of care for older persons and the first resort when health fails, the formal health care system exists for when there are no informal caregivers available or when the demands exceed seniors’ capacity to cope on their own. Three decades of research have demonstrated that, in addition to supporting informal caregivers, a society must have long-term home care (Chappell 2009) to address the challenges of an aging population. The aim of these services is to support the individual in optimizing function and quality of life, while minimizing the loss of independence. Clark (2007) notes that home care, as defined by Health Canada, has “an array of services which enables clients, incapacitated in whole or in part, to live at home, often with the effect of preventing, delaying, or substituting for long-term care or acute care alternatives.” The three functions of home care are to substitute for more costly acute care services and residential care in nursing homes, to maintain clients’ independence and to prevent functional decline for as long as possible. While the federal government provides support for home care through general transfer payments for health and social services, home care services depend on each province and territory.
In Canada, medicare, while universal, includes only hospital and physician care. It is well documented that its establishment ensured these services are available to all based on need, and not on economic ability (barring some exceptions: for example, rural and remote areas often do not have ready access to these services) (Manga 1978; Broyles et al. 1983). But other health care services are not universally available. Home care and home support services, nursing home care, and practitioners such as chiropractors, naturopaths, physiotherapists and dentists as well as prescription drugs (except in an acute care hospital) are outside of medicare. In fact, coverage varies with the province of residence as to what services are covered, whether user fees are charged, whether physician referral is required and other conditions.
The relevance for older adults lies in the fact that in old age, we suffer primarily from chronic conditions for which medicine has no cure; they primarily require long-term non-physician care. The care required, though, is prompted by medical need. Also, older adults, like younger and middle-aged adults, prefer to remain in their own homes while receiving needed care rather than being institutionalized.
The importance of the formal care sector may become ever greater in the next few decades as there is a growing concern that lower fertility rates will result in less availability of family caregivers. Indeed, some literature, although it is not abundant, suggests that childlessness among either single or married persons is related to the receipt of less informal support. Larsson and Silverstein (2004) project a steady increase in the proportion of older women who do not have surviving children, potentially translating into less available support (see also Keefe, forthcoming). Especially from 2021 onward, the proportion of women over age 85 with no surviving children will rise significantly.
Moreover, increasing rates of divorce and remarriage and the increasing number of blended families may affect the provision of care by children. There is much that remains unknown about these newer family forms, and about new social arrangements that may arise and replace the “traditional” family network. For instance, Grossman, D’Augelli and Hershberger (2000) record lesbian, gay and bisexual couples and individuals as having diverse and rich social networks with various kinds of informal support. In addition, while baby boomers have fewer children, they have more siblings who could step in to provide care. And as the gender gap in both longevity and societal roles decreases, more husbands may provide care in the future.
Even if the proportion of seniors requiring formal assistance remains stable, the increase in the actual number of seniors means that there will be an absolute and a relative increase in the need for formal support. The issue is relevant both to older adults themselves and to their family caregivers, especially given that many seniors receive both formal and informal care. In jurisdictions without specific services, with limited services and/or with charges for services, both caregivers and seniors suffer: when needed services are not available or too costly, demands increase on family members because there is no alternative, and older adults without informal support must go without care.
Past and current research supports the establishment of a comprehensive, long-term home care system and also raises questions about the assumption that prevailed when medicare was established: that medicine is the most appropriate means to ensure the health of the nation. For example, McKeown, Record and Turner (1975) early on demonstrated that widespread medical intervention began after 92 percent of the modern decline in mortality occurred, except for the eradication of smallpox, which accounted for about 5 percent of the reduction. These authors attributed the decline in mortality to public health measures and rising standards of living, such as improved diet and hygiene and increased natural immunity and nutrition. Almost two decades later, Badgely (1991) concluded, after a review of Canadian research, that the gap between rich and poor in longevity and in the prevalence of illness had improved little since the introduction of medicare. At that time, reports also appeared suggesting that the principal factors for enhancing the health of the population are not related to health care. The General Accounting Office in the United States (1991), for example, noted that only 10 percent of premature deaths were attributable to inadequate health care services; 50 percent were due to unhealthy lifestyles, 20 percent to environmental factors and 20 percent to biological factors. Medicine, in other words, was not the main engine for promoting health or preventing disease, however important it is for curing many ailments after they arise. Furthermore, by definition, medicine cannot cure chronic illnesses, the major concern during old age.
Recent research examining the needs of older adults demonstrates the cost-effectiveness of home care. Hollander (2001) studied the preventive function of home care in two health units that implemented cuts only to homemaking services as directed by the B.C. government in the 1990s and in two health units that did not do so. Individuals who had homemaking services withdrawn cost the government more in terms of hospital beds, home care services and admissions to nursing homes in the second and third years after the cuts. Hollander and Chappell (2002) and Chappell and colleagues (2004), in separate studies, measured the costeffectiveness of home care for older adults: home care was 40 percent to 75 percent less expensive than institutional facility care, depending on the level of care examined. The only time that the costs associated with home care clients exceeded those of nursing care clients was when individuals died while in home care, and those higher costs were attributable to hospitalization at the end of life, not to home support services. In fact, the cost-effectiveness of long-term home care relative to institutional care for older adults is one of the key arguments for expanding Canada’s long-term community care system (Hollander et al. 2007).
The vision of health care that emerged in the 1990s and was embraced by virtually all of the federal and provincial task forces and committees at the time encompassed such a system, as more cost-effective and more appropriate for an aging society (Mhatre and Deber 1992). The National Forum on Health (1997) report, chaired by the prime minister of the day, Jean ChreÌtien, recognized home care as a medically necessary service, recommending that it, along with prescription drugs, be included in publicly funded medicare (neither has yet been added). That report, like others at the time, embraced a broad definition of health that went beyond the absence of disease (i.e., biomedicine); bringing services closer to home (i.e., not concentrating them within acute care hospitals); health promotion and disease prevention in addition to cure; and ensuring citizens have more say. The notion that good health requires a clean, safe environment; adequate income; meaningful roles in society; and good housing, nutrition, education and social support was also supported. This vision embraced basic values endorsed by most Canadians: equity, compassion, collective responsibility, individual responsibility, respect for others, efficiency and effectiveness (National Forum on Health 1997).
However, the reforms implemented in Canada throughout and since the 1990s have not created a health care system that is more appropriate for an aging society. Rather, there has been a hollowing-out of medicare, whereby health services are increasingly provided outside of the medicare or hospital system. Because health services that are neither strictly medical nor provided within hospitals are usually not publicly insured, they are open to the private sector (Williams, Deber and Gildiner 2001). This is exemplified by the rise in private expenditures reported by Le Goff (2002), albeit only for one year: per capita private expenditures allocated to home care increased by 18.6 percent from 1999-2000 to 2000-2001, while public provincial expenditures increased by 3.9 percent in the same period.
Furthermore, research by Penning, Allan and Brackley (2001) and Penning, Brackley and Allan (2006) suggests the dismantling of long-term home care or support services for older adults has slowly been taking place since the 1970s and 1980s. That is, health care reform begun in the 1990s and continuing today did not initiate but rather saw a continuation of the dismantling process. Their results reveal fewer people receiving long-term home care and the intensification of care for targeted beneficiaries — those in need of higher levels of care and more hours of service — throughout the 1990s. There appears to be a redirection of services away from those in less need (who are potentially good candidates for prevention of disease and disability) to more intensive, medically focused post-acute care.
The lack of universally available services has known consequences for specific groups — those with fewer socio-economic resources, women, and disadvantaged race and ethnic groups — who suffer most because of structural forces that intersect to create disadvantage on multiple aspects of care need and care provision (the need for care, the resources for securing the needed care, the location of care, the type and level of care, and care provision) (Chappell and Penning 2005; Glaser and Grundy 2002). This is summarized by Chappell and Penning (2005) when discussing trends toward the commodification of care within current health care reform in Canada and disadvantaged groups within society:
The results can easily be predicted and include disproportionate increases in unmet needs, spend down of private economic resources, and intensification of personal and familial responsibilities for care provision. This, in turn, can be expected to generate repercussions for the employment, income, health and well-being of those assuming such responsibilities. Ultimately, therefore, one can expect such trends not only to reinforce but also, to amplify existing structural inequalities of gender, ethnicity, race and class. (461)
More specifically, over the last decade or so, two broad trends have affected the development of home care services in Canada. Increasing demands are being made on home care services, due to the growing older adult population and the increasing number of outpatient surgeries that have increased demand for short-term home care services such as rehabilitation, prescription drugs, nursing and custodial care. Over the 10-year period 1995-96 to 2005-06, the total number of days in acute care hospitals decreased by 13 percent; hospital admissions decreased by 25 percent (CIHI 2007). This shift toward shorter hospital stays and day surgeries (Deber et al. 1998) has increased demand for post-acute home support, which necessitates intensive and expensive home care compared with long-term chronic home care for seniors. As noted in a report to the Annual Premiers’ Conference as early as 2002, increased demand for short-term home care services due to increased incidence and acuity of care has led to a change in the mix of services at the expense of long-term home care, which is more suited to the needs of older adults (see Special Senate Committee on Aging 2009).
While public budgets for home care (estimated to constitute 88 percent of all monies spent on home care) increased 12.9 percent annually from 1994-95 to 1998-99, they decreased thereafter by 3.4 percent in 2000-01 and by 0.7 percent in 2003-04. During this time, the per capita spending increased more rapidly than the number of users, suggesting more intensive use per client. In some provinces, notably Saskatchewan and British Columbia, the number of users decreased (CIHI 2007). Furthermore, home care allocations constitute only between 2 percent and 4 percent, depending on the estimate, of public expenditures on health care (CIHI 2003; Canadian Home Care Association 2004), so small a proportion that it does not warrant its own category in reports on national health expenditures compiled by CIHI (2009).
Examining data from the 1994-95 National Population Health Survey and the 2003 Canadian Community Health Survey, Kathryn Wilkins reports that the average age of government-subsidized home care recipients fell from just under 65 to 63 years old and that the proportion of very old Canadians receiving such services also declined, from 22 percent to 19 percent. Most significantly, the proportion of recipients receiving nursing care services increased from 39 percent to 52 percent, while the proportion of those receiving household support services declined from 51 percent to 33 percent (Wilkins 2006).
Data from the Canadian Institute for Health Information (CIHI 2007) confirm this trend. The institute examined public sector expenditures on home care and showed that the health component is accounting for an increasingly large share of home care spending, compared with home support services: it grew from 43.3 percent in 1995-96 to 48.6 percent in 2003-04. In the seven jurisdictions for which data are available, the average annual change in real per capita spending (in constant 1997 dollars) on the health component of home care was almost 6 percent between 1995-96 and 2003-04, compared with 3 percent for home support services; the gap would likely be greater if New Brunswick were removed from the average, as it is the only province where the increase in home support was larger than for health care (almost 9 percent compared with almost 3 percent respectively).5 Finally, CIHI also reports that the number of users of “government-subsidized” home care services per 1,000 population was estimated at 26.1 in 2003, an average annual increase of only 1 percent compared with the 1994-95 level. This suggests that, in general, each home care user consumed more resources in 2003 than he or she did previously. Thus, home care is becoming more a medical support system than one providing chronic care, representing a major shift in service provision for older adults.
Another trend in the development of home care services is the shift to a mixed mode of managed competition or quasi markets in most provinces, in a move to commodify services and regulate them using market principles (Manitoba stands as an exception). Local health authorities often purchase services from a mix of not-for-profit and for-profit service providers on behalf of consumers. The rationale is to keep costs down through competition, seemingly ignoring the evidence suggesting that for-profit firms are more likely to skimp on quality and increase profits by selecting those clienteles that are in the least need (Bendick 1989; Williams, Deber and Gildiner 2001). While research in the United Kingdom on managed competition for home care has been unable to find measurable change (Le Grand 1999), research in the United States about for-profit health maintenance organizations reveals cherry-picking of only healthy or low-risk clients and threats to access and quality of care (Newhouse, Buntin and Chapman 1997; Kronick and DeBeyer 1997).
Although for-profit health care can be less expensive for governments, it is more expensive for consumers (Canadian Healthcare Association 2009), and profits go to owners and stakeholders rather than being invested back into the care that is delivered. That is, not only can for-profit care be more costly for consumers but also less quality of care can result. In Canada, Abelson and her colleagues (2004) noted, after studying competitive contracting for home care services in Ontario, that the complexity of the home care sector, together with measurement challenges and human resource uncertainties, affects the achievement of efficiencies typically expected in the marketplace. They go on to argue that such a model can contribute to inefficiency of resource use through discontinuous care to clients and disruption to collaborative relationships among different care providers, confirming research by others (Brown and Potoski 2003; Flynn, Williams and Pickard 1997). Interestingly, Manitoba reverted back to publicly provided home care after a one-year trial period when service provision proved more expensive than publicly delivered services and resulted in an increase of the staff turnover rate, from 15-25 percent to 50 percent (Shapiro 1997; Vogt et al. 2004).
In sum, despite recognition that an aging society is characterized by chronic conditions most appropriately requiring long-term community care, largely although not always non-medical in nature, only physician and acute care hospital services are provided universally in Canada. And health reforms, rather than changing direction, have consolidated a trend toward greater medicalization within medicare and more profitization of other health care services. As summarized by Clark (2007), the lack of action on the part of governments reflects overriding concerns with potential cost consequences, as they wrongly assume that the provision of formal public services to older adults and their caregivers will substitute for informal care and will impose overwhelming cost burdens on the public purse. This is in spite of cumulative evidence concerning the falsity of a substitution or “woodwork” effect (Clark 2007) (see note 6 for an explanation of the “woodwork effect”).6
If comprehensive long-term home care services are the most appropriate for an aging society (which is not to argue that acute care medical services are not also needed at times), how can and should they be established?
Two options proposed in the past are adopting separate legislation relating specifically to long-term community care or adding this service to medicare. (The Canada Health Act does not define health care as only medical care — physician care and care in acute care hospitals — but that was the interpretation when it was implemented.) The first was recommended by the Canadian Healthcare Association (2009), which also urged the federal government to adopt a strong role in this area, as many reports over the last several years have also said (Clark 2007). The second was recommended by the National Forum on Health in 1997. The Commission on the Future of Health Care in Canada (Romanow 2002) also appealed to the values that underlie medicare — equity, fairness and solidarity — when describing a national home care policy as the next essential service. Both options considered that the ability to pay should not be the basis for accessing appropriate and needed care. However, Romanow’s recommendations included only short-term home care, specifically focusing on three areas for priority: mental health, post-acute care and palliative care. The First Ministers’ Accord, signed a year later (Health Canada 2003), also limited coverage to short-term services (acute home care services and a compassionate care benefit for family caregivers). The Health Council of Canada (2006) noted the short-term focus of the measures being implemented and recommended expansion of the “undervalued and underfunded” long-term and chronic home care system in Canada.
In addition to the need to create and sustain an adequate long-term community care system for older adults, the much maligned silos within the existing health care system require urgent attention. Calls have been heard for integration for years, and there are several efforts in this direction to improve quality of care, sustainability and access (Banks 2004). Indeed, integrated care delivery systems have been recommended as the most efficient and effective organization for care delivery for older adults (Hollander et al. 2007; Hollander and Prince 2002; MacAdam 2008). Without an integrated system, one that includes health and social support, home care, certain community services, case management, residential care, and some aspects of acute care (particularly continuing care), individuals fall through the cracks or cannot move easily from one service to the next, and cost-saving substitutions cannot easily be made.
Such a long-term integrated home care program also needs to link and partner with informal caregivers and with community voluntary and not-for-profit as well as for-profit organizations that may form the support network for informal caregivers and older adults. The formal health care system, in other words, should not remain isolated but must find ways to work with other individuals, groups and organizations to the benefit of older adults within the neighbourhoods in which they live. Integration is required both within as well as outside of the formal health care system.
Canada, like other countries, can provide care services to meet the needs of its growing older population if the will exists. But demands for care can be decreased if the need for care can be prevented through health promotion, which offers an important opportunity to reduce the care needs of older adults.
Canadians desire healthy aging to the extent possible. Health Canada (2002) defines healthy aging as “a lifelong process of optimizing opportunities for improving and preserving health and physical, social and mental wellness, independence, quality of life and enhancing successful lifecourse transitions.” Health promotion, the process of enabling people to increase control over and improve their health, has been embraced by several national reports, including that of the National Forum on Health (1997) and the Romanow commission (2002).
There is now a wealth of evidence demonstrating that many chronic conditions can be prevented and that it is cost-effective in human, social and financial terms to invest in policies to that effect (Kannus et al. 2005; Katz and Shah 2010; WHO, 2002; Heikkinen 2003). Smoking, lack of physical exercise and inadequate diet are established risk factors for virtually all chronic illnesses. For example, it is estimated that $1 put toward enhancing physical exercise results in a savings of $3.20 in medical costs (WHO 2002); $1 invested in health promotion has been estimated to yield a return on investment of $6 to $8 in health cost savings. A 20 percent decrease in falls experienced by older adults would result in 7,500 fewer hospitalizations, 1,800 fewer permanently disabled older adults and a cost saving of $138 million a year in health care costs (PHAC 2009). Prevention takes us squarely to areas outside of strict physiology to include cognitive abilities, personal health behaviours, and psychological and social factors. It takes us to the area of the distribution of a country’s resources, to differences in socio-economic status and to the fact that the gap between the rich and the poor is increasing in all parts of the world — and so too, as a related effect, are disparities in health status and overall inequality (Lynch et al. 2000; Paton 2009; Navarro 2007). In short, it takes us to the social determinants of health. Without reiterating here the widespread literature on the social determinants of health, it can be noted that health promotion efforts direct attention to the very structure of society and the current socio-economic disparities that affect the lifelong experience of many individuals. Addressing these issues ultimately requires the involvement of all levels of government, civil society and local communities, businesses, and international agencies. It involves daily living conditions, education, the built and natural environments, fair employment and decent work, and social protection.
Specifically in relation to older age, prevention includes valuing older adults within society and ensuring meaningful roles for their participation — perhaps, but not necessarily, including employment. The end of mandatory retirement can be seen as a step in the right direction in that it allows individuals the choice to remain within the labour force; on the other hand, pension policies in the future are likely to begin full benefits at a later age, so it will mean that those without economic resources will be required to continue working. Even though older adults represent a wealth of experience and a huge resource, ageism remains a barrier to their full participation in society. In virtually all walks of life, visible signs of aging are associated with devaluation and an assumption that declines in physical health reflect diminished internal capacity (Clarke and Griffin 2008). The labour force is but one example. Discrimination against older workers continues, despite increasing recognition that the workforce will shrink as the baby boom generation retires. Whether these attitudes will change as employers encounter future labour shortages is unknown.
A related area is human resources: employment opportunities in working with older adults, a growth area currently and in the future. Yet it is difficult to attract individuals to work in jobs with older adults, especially caring for older adults. Among those who are employed in such fields, there is evidence that discriminatory attitudes are reflected in how they perform their work (Gonçalves 2009). For example, Kane, Lacey and Green (2009) find that social work students perceive older adults as vulnerable, marginalized, only moderately resilient in overcoming depression or substance abuse and unlikely to seek professional help. The need to change attitudes toward older adults generally has been recognized by the Special Senate Committee on Aging (2009), which recommended that the federal government take a lead in an aggressive public relations campaign to portray seniors in a positive light. Without a valued role as contributing members of society, older adults’ selfworth and ultimately health and well-being are undermined.
Policies supporting social networks for older adults are also part of the health promotion agenda through, for instance, supporting community groups run by older people, volunteering, neighbourhood helping, peer mentoring and visiting, family caregivers, and intergenerational programs in outreach services (WHO 2002).
The WHO’s Age-Friendly Cities (now Communities) initiative is an example of a health promotion program embracing multiple levels of change. In 2002, the WHO launched its Active Ageing Policy Framework, defining active aging as “the process of optimizing opportunities for health, participation and security in order to enhance quality of life as people age” (Kalache 2009). For WHO, active aging requires a variety of supports including personal, physical environmental, economic, behavioural, and health and social services. WHO’s Global Age-Friendly Cities guide was launched in 2007, targeting eight domains for action: outdoor spaces and buildings; transportation; housing; social participation; respect and social inclusion; civic participation and deployment; communication and information; and community support and health services.7 Enabling policies, ones that encourage the restoration of function and expansion of participation of older people in all aspects of society, are age-friendly policies. They include barrier-free workplaces; welllit streets; exercise programs; lifelong learning and literacy programs; hearing aids and instruction in sign language; barrier-free access to health centres; credit schemes and access to small business; and changed attitudes of health and social service providers toward older adults. The Special Senate Committee on Aging (2009) recommends that the federal government promote the WHO’s Global Age-Friendly Cities guide (2007) and the Age-Friendly Rural and Remote Communities Guide (Federal/Provincial/Territorial Committee 2009). Thus far, four provinces are championing age-friendly communities (British Columbia, Manitoba, Nova Scotia and Quebec) (PHAC 2011).
While the challenges loom large, the potential payoff of illness prevention is great. It represents the possibility of reducing the care needs of older adults. Yet, at the present time, less than 3 percent of public health care funding is directed toward health promotion and disease prevention (PHAC 2010). Like other industrialized nations, Canada is struggling with the implementation of health promotion and disease prevention programs that draw on our knowledge of the social determinants of health. Incorporating structural elements together with individualand organizational-level interventions has proven far from easy.
Currently, health promotion and illness prevention initiatives typically entail little more than the provision of information about healthy lifestyle, such as proper nutrition or the harmful effects of excessive alcohol consumption or smoking (Chappell 2009). Presumably one of the stumbling blocks to broader social policies relating to health promotion is that they fall outside of the health care system and therefore encounter jurisdictional challenges in a system where administrative silos abound (Canada 2010). How to handle cross-cutting responsibility with different levels of government is yet to be pursued, let alone answered. No doubt the longer time spans required in order to see the results of health promotion programs are also a stumbling block because of the lack of immediate and clear-cut results.
The challenge therefore is to implement policies that provide opportunities for lifelong learning and encourage it, educating the workforce in both the health care and civil service sectors; to embrace a health promotion perspective, including the social determinants of health; and to collaborate across government jurisdictions to ensure cross-cutting issues are acted upon.
This paper presents the evolving needs and the main health and social policy challenges raised by population aging in three areas: informal care, formal care and prevention. Although the discussion has focused on long-term care, this is a sector that covers a vast territory. This paper thus necessarily presents an overview of only some of the relevant points.8
At present, and throughout history, the dominant care system is the informal network consisting primarily of family members, mostly wives and daughters who care for elderly spouses and parents as the need arises. Despite the many documented demands and burdens of this role, and the sacrifices made in order to provide care, family members are not, contrary to what is often believed, seeking to relinquish this caring role. Nevertheless, demands sometimes become overwhelming, putting caregivers at risk of their own health deteriorating, not to mention potentially putting the older adult at risk through the lack of proper care. Yet there are few formal services targeted to caregivers; historically the health care system directs resources to the older adults, not the caregiver. Despite the many calls for the federal government to take a leadership role in establishing formal support for caregivers, to date help has not been forthcoming.
Long-term home care within the community, allowing the vast majority of older adults in need to remain in their own homes, has been advocated by gerontologists for several decades as the service system of choice in old age. It has been recognized in several national reports on Canada’s health care system as the next essential service that should be added to medicare. But this has not yet occurred either. Older Canadians needing home care today are faced with a patchwork of services that vary from jurisdiction to jurisdiction, are typically means-tested and are delivered through mixed modes of services that include both not-for-profit and for-profit agencies. Moreover, health care reform that is increasing the number of outpatient surgeries is increasing the demand for more short-term, intensive post-hospital home care, which current evidence suggests is redirecting resources away from long-term home care at a time when the size and care needs of Canada’s elderly population are increasing.
Hence the challenge is to establish a comprehensive community care system to ensure that necessary health and support services are provided based on needs and to recognize informal caregivers in the process. In order to do so, Canada requires a debate on how to best accomplish this goal. Should the system be universal? How should the needs of caregivers be taken into account? How can families and neighbourhood and community organizations partner in order to coordinate the best care possible? What services should be included? What eligibility criteria should be applied? How much of each should be funded? How can such a system be established so it is both appropriate and cost-effective? How can an integrated system be established so that comprehensive home care will not represent a cost add-on?
One option is to target specific at-risk groups such as the very old, the frail or single older women. Such strategies inevitably include some who do not require care and miss some who do (Penning and Chappell 2010; Chappell and Penning, forthcoming). If services are provided based on need, with appropriate needs assessments, those in need are the ones who receive the care. Assessments ensure there will not be an opening of the floodgates; rather, services go where they are needed.
In pursuing answers to these questions, it is imperative that beliefs and assumptions be made explicit and evidence be fairly adjudicated. To date, much evidence is ignored on the sustainability of universal, public systems of care; the greater cost of care in for-profit delivery; as well as the cost-effectiveness of home care compared with institutional care. In other words, policies and programs are put in place without evidence of their appropriateness or effectiveness. For example, we lack evidence that many of the interventions in current use have increased quality of life or prevented a decline (such as the use of cholinesterase inhibitors in the treatment of dementia or, as many reports have pointed out, the increased use of diagnostic tests in older adults). It is also imperative that issues beyond the scope of this paper — such as increased technological innovations and pharmaceutical intervention that are known cost drivers — be tackled. It is essential that the broader issue of increased medical intervention be addressed. An independent council or some other mechanism for assessing effectiveness of interventions could be put in place, as recommended by Romanow (2002). The issue of evidence-based medical practice, which bases practice and funding on scientifically demonstrated effectiveness, cannot be ignored if the goal is a cost-effective and appropriate health care system for an aging society.
Ideally, one wants to decrease the illness and disability that accompany old age. This is the promise of health promotion. Unfortunately, despite increasing recognition of the importance of health promotion and illness prevention strategies, health reforms begun in the 1990s have been dominated by a focus on physician and hospital services, particularly the latter. Little attention has been directed to larger structural elements of the community, such as the workplace and education institutions where health promotion takes place. The recognition of the social determinants of health and the necessity for multilevel, multifaceted initiatives provides direction for potentially making gains not on one disease or disability but on many simultaneously. However, the complexity of the programming required suggests basic structural change at the societal level will be necessary, which will require extraordinary political will. Whether many small and largely uncoordinated efforts will achieve significant change is unknown, but it seems unlikely. In developing policy in the prevention and health promotion area, debate is required on how best to combat ageism and replace it with realistic positive images of ageing, recruit more human resources to work with older adults, facilitate agefriendly communities, and combat poverty and social isolation.
The fact that not everyone in older age requires care or requires heavy care suggests energy should not be wasted worrying about excessive demands. Rather, focus should be placed on ways in which appropriate care can be provided to those in need. This paper indicates that the most appropriate care system for an aging society is one that supports both caregivers and older adults in a comprehensive long-term home care system. Such a system can be cost-effective if established so that it substitutes for more expensive forms of other services when care needs justify it. The good news is that there are known alternatives to provide appropriate and cost-effective care to an aging society. Whether Canada will move in that direction remains to be seen.
Abelson, J., S.T. Gold, C. Woodward, D. O’Connor, and B. Hutchison. 2004. “Managing under Managed Community Care: The Experiences of Clients, Providers and Managers in Ontario’s Competitive Home Care Sector.” Health Policy 68 (3): 359-72.
Achenbaum, W.A. 1995. Crossing Frontiers: Gerontology Emerges as a Science. New York: Cambridge University Press.
Alberta. 2008. Office of Statistics and Information. “Sex Ratio, Total Dependency Ratio and Aging Index Alberta and Canada, 2001 and 2006.” Fact sheet. Accessed October 1, 2011. https://osi.alberta.ca/osi-content/Pages/Factsheets/ SexRatio,TotalDependencyRatioandAgingIndex,AlbertaandCanada.aspx
—————–. 2009. Agriculture and Rural Development. “The Demographic Shift.” Accessed September 23, 2011. https://www1.agric.gov.ab.ca/$department/deptdocs.nsf/all/csi12639
Annual Premiers’ Conference. 2002. Strengthening Home and Community Care across Canada: A Collaborative Strategy. N.p.
Andren, S., and S. Elmstahl. 2005. “Family Caregivers’ Subjective Experiences of Satisfaction in Dementia Care: Aspects of Burden, Subjective Health and Sense of Coherence.” Scandinavian Journal of Caring Sciences 19 (2): 157-68.
Badgely, R.F. 1991. “Social and Economic Disparities under Canadian Health-Care.” International Journal of Health Services 21 (4): 659-71.
Bakas, T., and S.C. Burgener. 2002. “Predictors of Emotional Distress, General Health, and Caregiving Outcomes in Family Caregivers of Stroke Survivors.” Topics in Stroke Rehabilitation 9 (1): 34-45.
Banks, J.A. 2004. “Teaching for Social Justice, Diversity, and Citizenship in a Global World.” Educational Forum 68(4): 296–305.
Barer, M.L., R.G. Evans, and C. Hertzman. 1995. “Avalanche or Glacier?” Canadian Journal on Aging 14 (2): 193-224.
Bendick, M., Jr. 1989. “Privatizing the Delivery of Social Welfare Services: An Ideal to Be Taken Seriously.” In Privatization and the Welfare State, edited by S.B. Kamerman and A.J. Kahn. Princeton, NJ: Princeton University Press.
Braithwaite, V. 1998. “Institutional Respite Care: Breaking Chores or Breaking Social Bonds?” Gerontologist 38 (5): 610-17.
Brown, T.L., and M. Potoski. 2003. “Managing Contract Performance: A Transaction Cost Approach.” Journal of Policy Analysis and Management 22 (2): 275-97.
Broyles, R.W., P. Manga, D.A. Binder, D.E. Angus, and A. Charette. 1983. “The Use of Physician Services under a National Health Insurance Scheme.” Medical Care 21: 1037-54.
Calasanti, T.M., and K.F. Slevin. 2001. “Gender, Care Work and Family in Old Age.” In Gender, Social Inequalities and Aging, edited by T.M. Calasanti and K.F. Slevin. Walnut Creek, CA: Altamira Press.
Canada. 2006. The Human Face of Mental Health and Mental Illness in Canada. Ottawa: Public Works and Government Services Canada.
Canada. 2010. “New Horizons for Seniors Program – Federal Elder Abuse Initiative Funding Guide.” Ottawa: Human Resources and Skills Development Canada.
Canadian Caregiver Coalition. 2008. A Framework for a Canadian Caregiver Strategy: A Canada That Recognizes and Respects the Integral Role of Family Caregivers in Society. Acessed September 23, 2011. https://www.albertacaregivers.org/pdf/ CCCFramework.pdf
Canadian Health Services Research Foundation (CHSRF). 2001. “Myth: The Aging Population Will Overwhelm the Healthcare System.” Mythbusters series. Ottawa: CHSRF.
Canadian Healthcare Association. 2009. Homecare in Canada: From the Margins to the Mainstream. Ottawa: the Association.
Canadian Home Care Association. 2004. Realizing the Potential of Home Care. Accessed September 23, 2011. https://www.cdnhomecare.ca/media.php?mid=464
Canadian Institute for Health Information (CIHI). 2003. “Rate of Hospitalizations Continues to Decline but Average Length of Stay Is Increasing Slightly.” Media release November 19. Ottawa: CIHI.
—————–. 2007. Public-Sector Expenditures and Utilization of Home Care in Canada: Exploring the Data. Ottawa: CIHI. Accessed September 23, 2011. https://secure.cihi.ca/cihiweb/products/trends_home_care_mar_2007_e.pdf
—————–. 2009. “Most, but Not All, Canadians with Chronic Conditions Get Clinically Recommended Tests.” Media release July 23. Ottawa: CIHI.
—————–. 2011a. Seniors and the Health Care System: What Is the Impact of Multiple Chronic Conditions? Ottawa: CIHI. Accessed September 23, 2011. https://secure.cihi.ca/cihiweb/products/air-chronic_disease_aib_en.pdf
—————–. 2011b. “Health Indicators 2011.” Ottawa: CIHI. Accessed October 18, 2011. https://secure.cihi.ca/cihiweb/ products/health_indicators_2011_en.pdf
Canadian Study of Health and Aging Working Group. 1994. “The Canadian Study of Health and Aging: Study Methods and Prevalence of Dementia.” Canadian Medical Association Journal 150: 899-913.
Canuscio, C., J. Jones, I. Kawachi, G. Colditz, L. Berkman, and E. Rimme. 2002. “Reverberations of Family Illness: A Longitudinal Assessment of Informal Caregiver and Mental Health Status in the Nurses’ Health Study.” American Journal of Public Health 92 (8): 1305-11.
Chappell, N.L. 2007. “Aging among Chinese Canadian Immigrants – Reflections.” In Reading Sociology: Canadian Perspectives, edited by L. Tepperman and A. Kalyta. Don Mills, ON: Oxford University Press.
—————–. 2008. “Comparing Caregivers to Older Adults in Shanghai.” Asian Journal of Gerontology and Geriatrics 3 (2): 57-65.
—————–. 2009. “The Way Ahead.” In Health and Aging in British Columbia: Vulnerability and Resilience, edited by D. Cloutier-Fisher, H. Foster, and D. Hultsch. Canadian Western Geographical Series, 43. Victoria, BC: Western Geographic Press.
Chappell, N.L., and A.A. Blandford. 1991. “Informal and Formal Care: Exploring the Complementarity.” Aging and Society 11 (3): 299-317.
Chappell, N.L., and H.A. Cooke. 2010. “Age Related Disabilities – Aging and Quality of Life.” In International Encyclopedia of Rehabilitation, edited by J.H. Stone and M. Blouin. Center for International Rehabilitation Research Information and Exchange, University at Buffalo, SUNY; Laboratoire d’informatique et de terminologie de la réadaptation et de l’intégation sociale , Institut de réadaptation en déficience physique de Québec. Accessed September 23, 2011. https://cirrie.buffalo.edu/encyclopedia/en/article/189/
Chappell, N.L., and C. Dujela. 2008. “Caregiving, Predicting At-Risk Status.” Canadian Journal on Aging 27 (2): 169-79.
Chappell, N.L., and L.M. Funk. Forthcoming. “Social Support and Aging in Canada — Revisited.” Canadian Journal on Aging.
Chappell, N.L., B. Havens, M.J. Hollander, J. Miller, and C. McWilliam. 2004. “Comparative Costs of Home Care and Residential Care.” Gerontologist44 (3): 389-400.
Chappell, N.L., and K. Kusch. 2007. “The Gendered Nature of Filial Piety — A Study among Chinese Canadians.” Journal of Cross-Cultural Gerontology 22: 29-45.
Chappell, N.L., L. MacDonald, and M. Stones. 2008. Aging in Contemporary Canada. 2nd ed. Toronto: Pearson Educational.
Chappell, N.L., and M.J. Penning. 2005. “Family Caregivers in the Context of Health Reform.” In The Cambridge Handbook of Age and Aging, edited by M. Johnson. Cambridge, UK: Cambridge University Press.
Chappell, N., and M.J. Penning. Forthcoming. “Health Inequalities in Later Life, Differences by Age/Stage.” Paper prepared for the Public Health Agency of Canada. March.
Chappell, N.L., and R.C. Reid. 2002. “Burden and Well-Being among Caregivers: Examining the Distinction.” Gerontologist 42 (6): 772-80.
Chappell, N.L., R.C. Reid, and E. Dow. 2001. “Respite Reconsidered: A Typology of Meanings Based on the Caregiver’s Point of View.” Journal of Aging Studies 15 (2): 201-16.
Christakis, N.A., and P.D. Allison. 2006. “Mortality after the Hospitalization of a Spouse.” New England Journal of Medicine 354 (730): 719-30.
CHSRF (see Canadian Health Services Research Foundation).
CIHI (see Canadian Institute for Health Information).
Clark, P.G. 2007. “Understanding Aging and Disability Perspectives on Home Care: Uncovering Facts and Values in Public-Policy Narratives and Discourse.” Canadian Journal on Aging 26 (supplement 1): 47-62.
Clarke, L.H., and M. Griffin. 2008. “Visible and Invisible Ageing: Beauty Work as a Response to Ageism.” Ageing and Society 28: 653-74.
Cranswick, K. 2003. General Social Survey, Cycle 16: Caring for an Aging Society. Ottawa: Statistics Canada.
Dannefer, D., P. Stein, R. Siders, and R.S. Patterson. 2008. “Is That All There Is? The Concept of Care and the Dialectic of Critique.” Journal of Aging Studies 22: 101-8.
Deber, R., L. Narine, P. Baranek, N. Sharpe, K.K. Duvalko, R. Zlotnik-Shaul, P. Coyte, G. Pink, and A.P. Williams. 1998. “The Public-Private Mix in Health Care.” In Striking a Balance: Health Care Systems in Canada and Elsewhere, Vol. 4. Commissioned by the National Forum on Health. Quebec City: Editions MultiMondes.
Denton, F.T., C.H. Feaver, and B.G. Spencer. 1998. “The Future Population of Canada, Its Age Distribution and Dependency Relations.” Canadian Journal on Aging 17: 83-109.
Denton, F.T., and B.G. Spencer. 1999. Population Aging and Its Economic Costs: A Survey of the Issues and Evidence. SEDAP Research Paper No. 1. Hamilton, ON: McMaster University. Accessed September 23, 2011. https://socserv2.mcmaster.ca/~sedap/papers99.htm
DesMeules, M., L. Turner, and R. Cho. 2004. “Morbidity Experiences and Disability among Canadian Women.”BMC Women’s Health 4 (supplement 1): S10, 1-10.
Di Matteo, L. 2005. “The Macro-Determinants of Health Expenditure in the United States and Canada: Assessing the Impact of Income, Age Distribution and Time.” Health Policy 71: 23-42.
Dossman, D., J. Fast, and N. Keating. 2005. Care Networks of Frail Seniors and the Formal-Informal Interface. Hidden Costs/Invisible Contributions Research Program. Edmonton: University of Alberta, Department of Human Ecology.
Federal/Provincial/Territorial Committee of Officials. 2009. Age-Friendly Rural and Remote Communities: A Guide. Accessed September 29. 2011. https://www.phac-aspc.gc.ca/seniors-aines/publications/public/healthy-sante/age_friendly_ rural/index-eng.php
Flynn, R., C. Williams, and S. Pickard. 1997. “Quasi-Markets and Quasi-Trust: The Social Construction of Contracts for Community Health Services.” In Contracting for Health: Quasi-Markets and the National Health Service, edited by R. Flynn and G. Williams. Oxford, UK: Oxford University Press.
Funk, L.M., and K.I. Stajduhar. 2009. Interviewing Family Caregivers: Implications of the Caregiving Context for the Research Interview. Qualitative Health Research, 19(6): 859-67.
Gee, E.M., and G.M. Gutman. 2000. The Overselling of Population Aging: Apocalyptic Demography, Intergenerational Challenges and Social Policy. Don Mills, ON: Oxford University Press.
Gilmour, H., and J. Park. 2006. “Dependency, Chronic Conditions and Pain in Seniors.” Health Reports 16 (supplement): 21-31.
Glaser, K., and E. Grundy. 2002. “Class, Caring and Disability: Evidence from the British Retirement Survey.” Ageing and Society 22: 325-42.
Gonçalves, D.C. 2009. “From Loving Grandma to Working with Older Adults: Promoting Positive Attitudes towards Aging.” Educational Gerontology 35: 202-25.
Grossman, A.H., R.D. D’Augelli, and S.L. Hershberger. 2000. “Social Support Networks of Lesbian, Gay and Bisexual Adults 60 Years of Age and Older.” Journals of Gerontology, Series B 55 (3): P171-P179.
Harrow, B.S., D.F. Mahoney, A.B. Mendelsohn, M.G. Ory, D.W. Coon, S.H. Belle, and L.O. Nichols. 2004. “Variation in Cost of Informal Caregiving and Formal-Service Use for People with Alzheimer’s Disease.” American Journal of Alzheimer’s Disease and Other Dementias 19: 299–308.
Health Canada. 2002. Workshop on Healthy Aging: Aging and Health Practices. Ottawa, ON: Health Canada, Division of Aging and Seniors.
—————–. 2003. First Ministers’ Accord on Health Care Renewal. Accessed October 17, 2011. https://www.hc-sc.gc.ca/
hcs-sss/delivery-prestation/fptcollab/2003accord/
index-eng.php
Health Council of Canada. 2006. Health Renewal in Canada. Toronto: Health Council of Canada.
—————–. 2008. Use of Home Care Services Funded by Government and Not Funded by Government: An Update on Primary Health Care and Home Care Renewal in Canada. Toronto: Health Council of Canada.
Heikkinen, E. 2003. What Are the Main Risk Factors for Disability in Old Age and How Can Disability Be Prevented? Health Evidence Network report. Copenhagen: WHO Regional Office for Europe. Accessed October 17, 2011. https://www.euro.who.int/document/E82970.pdf
Helliwell, J.F. 2003. “How’s Life? Combining Individual and National Variables to Explain Subjective Well-Being.” Economic Modelling 20 (2): 331-60.
Henderson, J., and L. Forbat. 2002. “Relationship-Based Social Policy: Personal and Policy Constructions of ‘Care’.” Critical Social Policy 22: 669-87.
Hill, G.B., W.F. Forbes, J. Lindsay, and I. McDowell. 1997. “Life Expectancy and Dementia in Canada: The Canadian Study of Health and Aging.” Chronic Diseases in Canada 18 (4): 166-7.
Hirst, M. 2005. “Carer Distress: A Prospective, Population-Based Study.” Social Science and Medicine 61 (3): 697-708.
Ho, S., A. Chan, J. Woo, P. Chong, and A. Sham. 2009. “Impact of Caregiving on Health and Quality of Life: A Comparative Population-Based Study of Caregivers for Elderly Persons and Noncaregivers.” Journals of Gerontology, Series A 64: 873-9.
Hogan, D.B. 2007. “Proceedings and Recommendations of the 2007 Banff Conference on the Future of Geriatrics in Canada.” Canadian Journal of Geriatrics 10 (4): 133-48.
Hogan, D.B., C. MacKnight, and H. Bergman. 2003. “Models, Definitions, and Criteria of Frailty.” Aging Clinical and Experimental Research 15 (supplement 3): 3-29.
Hollander, M.J. 2001. Final Report on the Comparative Cost Analysis of Home Care and Residential Care Services. Report prepared for the Health Transition Fund, Health Canada. BC: Hollander Analytical.
Hollander, M.J., and N.L. Chappell. 2002. Synthesis Report, Final Report of the National Evaluation of the Cost-Effectiveness of Home Care. Health Transition Fund, Health Canada. BC: Hollander Analytical.
Hollander, M.J., N.L. Chappell, M.J. Prince, and E. Shapiro. 2007. “Providing Care and Support for an Aging Population: Briefing Notes on Key Policy Issues.” Healthcare Quarterly 10 (3): 34-45.
Hollander, M.J., J. Miller, M. MacAdam, N.L. Chappell, and D. Pedlar. 2009. “Increasing Value for Money in the Canadian Healthcare System: New Findings and the Case for Integrated Care for Seniors.” Healthcare Quarterly 12 (1): 38-47.
Hollander M., and M.J. Prince. 2002. Analysis of Interfaces along the Continuum of Care. Victoria, BC: Hollander Analytic Services Inc.
Huguet, N., M.S. Kaplan, and D. Feeny. 2008. “Socioeconomic Status and Health-Related Quality of Life among Elderly People: Results from the Joint Canada/United States Survey of Health.” Social Science and Medicine 66: 803-10.
Kalache, A. 2009. “Towards Age-Friendly Societies: From Research to Policy, from Policy to Society.” International Journal of Integrated Care 9 (22).
Kane, M.N., D. Lacey, and D. Green. 2009. Investigating Social Work Students’ Perceptions of Elders’ Vulnerability and Resilience. London: Routledge.
Kane, R.L. 1990. “Introduction.” In Improving the Health of Older People: A World View, edited by R. Kane, J. Evans and D. MacFayden. New York: Oxford University Press.
Kannus. P., H. Sievanen, M. Palvanen, T. Jarvinen and J. Parkkari. 2005:. “Prevention of Falls and Consequent Injuries in Elderly People.” Lancet 366 (9500):1885-93.
Kaplan, M.S., N. Huguet, D.H. Feeny, and B.H. McFarland. 2010. “Self-Reported Hypertension Prevalence and Income among Older Adults in Canada and the United States.” Social Science and Medicine 70: 844-9.
Katz, R., and P. Shah 2010. “The Patient Who Falls.” Journal of the American Medical Association 303 (3): 273-4.
Keating, N., J. Fast, J. Frederick, K. Cranswick, and C. Perrier. 1999. Eldercare in Canada: Context, Content and Consequences. Catalogue No. 89-570-XPE. Ottawa: Statistics Canada, Housing, Family and Social Statistics Division.
Keefe, J. Forthcoming. “Who Will Care for Older Canadians? Caregiving Policy Challenges in the Short and Long Terms.” IRPP Study. Montreal: Institute for Research on Public Policy.
Keefe, J., and B. Rajnovich. 2007. “To Pay or Not to Pay: Examining Underlying Principles in the Debate on Financial Support for Family Caregivers.” Canadian Journal on Aging 26 (supplement 1): 77-90.
Kronick, R.T., and J. DeBeyer. 1997. Risk Adjustment Is Not Enough: Strategies to Limit Risk Selection in the Medicare Program. New York: Commonwealth Fund.
Lafrenière, S., Y. Carrière, L. Martel, and A. Belanger. 2003. “Dependent Seniors at Home: Formal and Informal Help.” Health Reports 14 (4): 31-40.
Lan, P.-C. 2002. “Subcontracting Filial Piety: Elder Care in Ethnic Chinese Immigrant Families in California.” Journal of Family Issues 23 (7): 812-35.
Langa, K.M., N.H. Fultz, S. Saint, M.U. Kabeto, and A.R. Herzog. 2002. “Informal Caregiving Time and Costs for Urinary Incontinence in Older Individuals in the United States.” Journal of the American Geriatrics Society 50: 733-7.
Langa, K.M., S. Vijan, R.A. Hayward, M.E. Chernewm, C.S. Blaum, M.U. Kabeto, D.R. Weir, S.J. Katz, R.J. Willis, and A.M. Fendrick. 2002. “Informal Caregiving for Diabetes and Diabetic Complications among Elderly Americans.” Journals of Gerontology, Series B 57 (3): S177–S186.
Larsson, K., and M. Silverstein. 2004. “The Effects of Marital and Parental Status on Informal Support and Service Utilization: A Study of Older Swedes Living Alone.” Journal of Aging Studies 18 (2): 231-44.
Lazar, H. Forthcoming. Many Degrees of Policy Freedom: The Federal Government’s Role in Care for Seniors. IRPP Study.
Le Goff, P. 2002. Home Care Sector in Canada: Economic Problems. Economics Division, Parliamentary Research Bureau. Accessed September 26, 2011. https://dsp-psd.pwgsc.gc.ca/Collection-R/LoPBdP/BP/prb0229-e.htm
Le Grand, J. 1999. “Competition, Cooperation, or Control? Tales from the British National Health Service.” Health Affairs 18 (3): 27-39.
Lindsay, C. 2008. “Do Older Canadians Have More Friends Now Than in 1990?” Matter of Fact no. 4. Statistics Canada cat. no 89-630-X. Accessed October 17, 2011. https://www.statcan.gc.ca/pub/89-630-x/2008001/article/10652-eng.pdf
Litwak, E. 1960. “Geographic Mobility and Extended Family Cohesion.” American Sociological Review25 :385-94.
Lynch, J.W., P. Due, C. Muntaner, and G.D. Smith. 2000. “Social Capital — Is It a Good Investment Strategy for Public Health?” Journal of Epidemiology and Community Health 54 (6): 404-8.
MacAdam, M. 2008. Frameworks of Integrated Care for the Elderly: A Systematic Review. Ottawa: Canadian Policy Research Networks (CPRN).
MacRae, H. 1998. “Managing Feelings: Caregiving as Emotion Work.” Research on Aging 20 (1): 137-60.
Magnus, G. 2009. The Age of Aging: How Demographics Are Changing the Global Economy and Our World. John Wiley and Sons (Asia), 2009.
Manga, P. 1978. The Income Distribution Effect of Medical Insurance in Ontario. Occasional Paper no. 6. Toronto: Ontario Economic Council.
Manton, K.G. 2008. “Recent Declines in Chronic Disability in the Elderly U.S. Population: Risk Factors and Future Dynamics.” Annual Review of Public Health 29: 91-113.
Martin-Matthews, A. 2000. “Change and Diversity in Aging Families and Intergenerational Relations.” In Canadian Families: Diversity, Conflict and Change. 2nd. ed. Edited by N. Mandell and J. Duffy. Toronto: Harcourt Canada.
McIntosh, C.N., P. Fines, R. Wilkins, and M.C. Wolfson. 2009. “Income Disparities in Health-Adjusted Life Expectancy for Canadian Adults, 1991 to 2001.” Health Reports 20 (4): 1-10.
McKeown, T., R.G. Record, and R.D. Turner. 1975. “An Interpretation of the Decline of Mortality in England and Wales during the Twentieth Century.” Population Studies 29 (3): 391-422.
Mendelson, M., and P. Divinsky. 2002. Canada 2015: Globalization and the Future of Canada’s Health and Health Care. Future of Global and Regional Integration project, Institute of Intergovernmental Relations. Caledon Institute for Social Policy.
Merette, M. 2002. “The Bright Side: A Positive View on the Economics of Aging.” IRPP Choices 8 (1).
Mhatre, S.L., and R.B. Deber. 1992. “From Equal Access to Health Care to Equitable Access to Health: A Review of Canadian Provincial Health Commissions and Reports.” International Journal of Health Services 22 (4): 645-68.
Morgan, S. and C. Cunningham. 2011. “Population Aging and the Determinants of Healthcare Expenditures: The Case of Hospital, Medical and Pharmaceutical Care in British Columbia, 1996 to 2006.” Healthcare Policy 7 (1): 68-79.
National Advisory Council on Aging (NACA). 2004. The NACA Position on Alzheimer Disease and Related Dementias. Ottawa: Minister of Public Works and Government Services Canada.
National Forum on Health. 1997. Canada Health Action: Building on the Legacy. Vol. I: The Final Report of the National Forum on Health and Vol. II: Synthesis Reports and Issue Papers. Ottawa: The Forum.
National Seniors Council. 2009. Report of the National Seniors Council on Low Income Among Seniors. Ottawa: Human Resources and Skills Development Canada. Accessed October 18, 2011. https://www.seniorscouncil.gc.ca/eng/ research_publications/low_income/2009/hs1_9/page00.shtml
Navaie-Waliser, M., P.H. Feldman, D.A. Gould, C. Levine, A.N. Kuerbis, and K. Donelan. 2002. “When the Caregiver Needs Care: The Plight of Vulnerable Caregivers.” American Journal of Public Health 92 (3): 409-13.
Navarro, V. 2007. Neoliberalism, Globalization and Inequalities: Consequences for Health and Quality of Life. Amityville, NY: Baywood.
Newhouse, J.P., M.B. Buntin, and J.D. Chapman. 1997. “Risk Adjustment and Medicare: Taking a Closer Look.” Health Affairs 16: 26-43.
O’Connor, D.L. 2007. “Self-Identifying as a Caregiver: Exploring the Positioning Process.” Journal of Aging Studies 21 (2): 165-74.
OECD (See Organisation for Economic Co-operation and Development)
Organisation for Economic Co-operation and Development. 2009. Health at a Glance 2009. Paris: OECD.
Ory, M.G., R.R. Hoffman, J.L. Lee, S. Tennstedt, and R. Schulz. 1999. “Prevalence and Impact of Caregiving: A Detailed Comparison between Dementia and Nondementia Caregivers.” Gerontologist 39 (2): 177-86.
Partridge, C., M. Johnston, and L. Morris. 1996. “Disability and Health: Perceptions of a Sample of Elderly People.” Physiotherapy Research International 1 (1): 17-29. Centre for Health Services Studies, University of Kent, Canterbury, UK.
Paton, C. 2009. Review of Fads, Fallacies and Foolishness in Medical Care Management and Policy, by T. Marmor. International Journal of Health Planning and Management 24 (1): 87-90.
Penning, M.J. 1998. “In the Middle: Parental Caregiving in the Context of Other Roles.” Journals of Gerontology, Series B 53 (4): S188-S197.
Penning, M.J., D.E. Allan, and M.E. Brackley. 2001. “Home Care and Health Reform: Changes in Home Care Utilization in One Canadian Province, 1990-1998.” Paper presented at International Association of Gerontology meetings, Vancouver.
Penning, M., M.E. Brackley, and D. Allan. 2006. “Home Care and Health Care Reform: Changes in Home Care Utilization in One Canadian Province, 1990-2000.” Gerontologist46 (6): 744-58.
Penning, M., and Chappell, N. 2010. “Health Inequalities among Adults in Later Life: Review of Issues, Promising Practices and Upstream Health Interventions in Responding to Aging and Older People in Canada.” Paper prepared for the Public Health Agency of Canada, June.
PHAC (see Public Health Agency of Canada)
Pickard, L. 2001. “Carer Break or Carer-Blind? Policies for Informal Carers in the UK.” Social Policy and Administration 35 (4): 441-58.
Pinquart, M., and S. Sörensen. 2003. “Associations of Stressors and Uplifts of Caregiving with Caregiver Burden and Depressive Mood: A Meta-analysis.” Journals of Gerontology, Series B 58 (2): P112-P128.
—————–. 2007. “Correlates of Physical Health of Informal Caregivers: A Meta-analysis.” Journals of Gerontology, Series B 62 (2): P126-P137.
Public Health Agency of Canada (PHAC). 2009. “Prevention of Unintentional Injuries among Seniors.” Accessed September 26, 2011. https://www.phac-aspc.gc.ca/seniors-aines/
publications/pro/healthy-sante/workshop-atelier/ injury/index-eng.php
—————–. 2010. “Age-Friendly Communities Initiative.” Accessed September 26, 2011. https://www.phac-aspc.gc.ca/sh-sa/ifa-fiv/2008/initiative-eng.php
—————–. 2011. “On the Road to Age-Friendly Communities.” Accessed September 26, 2011. https://www.phac-aspc.gc.ca/seniors-aines/publications/public/
healthy-sante/comm-coll/index-eng.php
Robison, J., R. Fortinsky, A. Kleppinger, N. Shugrue, and M. Porter. 2009. “A Broader View of Family Caregiving: Effects of Caregiving and Caregiver Conditions on Depressive Symptoms, Health, Work, and Social Isolation.” Journals of Gerontology, Series B 64 (6): 788-98.
Robson, W.B.P. 2001. “Will the Baby Boomers Bust the Health Budget? Demographic Change and Health Care Financing Reform.” C.D. Howe Institute Commentary 148 (February).
—————–. 2009. Boomer Bulge: Dealing with the Stress of Demographic Change on Government Budgets in Canada. C.D. Howe Institute. Accessed September 17, 2011. https://www.cdhowe.org/pdf/ebrief_71.pdf
Rockwood, K., and A. Mitnitski. 2007. “Frailty in Relation to the Accumulation of Deficits.” Journals of Gerontology, Series A 62 (7): 722-7.
Romanow, R. 2002. Building on Values: The Future of Health Care in Canada. Ottawa: Commission on the Future of Health Care in Canada.
Rosenmayr, L., and E. Kockeis. 1963. “Propositions for a Sociological Theory of Aging and the Family.” International Social Science Journal 15: 410-26.
Schulz, R., and S.R. Beach. 1999. “Caregiving as a Risk Factor for Mortality: The Caregiver Health Effects Study.” Journal of the American Medical Association 282: 2215-9.
Shapiro, E. 1997. The Cost of Privatization: A Case Study of Home Care in Manitoba. Ottawa: Canadian Centre for Policy Alternatives.
Sherwood, P.R., C.W. Given, B.A. Given, and A. von Eye. 2005. “Caregiver Burden and Depressive Symptoms: Analysis of Common Outcomes in Caregivers of Elderly Patients.” Journal of Aging and Health, 17 (2): 125-47.
Song, X., A. Mitnitski, and K. Rockwood. 2010. “Prevalence and 10-Year Outcomes of Frailty in Older Adults in Relation to Deficit Accumulation.” Journal of the American Geriatrics Society 58 (4): 681-7.
Special Senate Committee on Aging. 2009. Canada’s Aging Population: Seizing the Opportunity. Final Report. Ottawa: The Committee.
Statistics Canada. 2003. Canadian Community Health Survey. Accessed September 23, 2011. https://www.statcan.gc.ca/
cgi-bin/imdb/p2SV.pl?Function=getSurvey&SurvId= 3226&SurvVer=0&SDDS=3226&InstaId=15282&InstaVer=2&lang=en&db=imdb&adm=8&dis=2
—————–. 2007. “Seniors Satisfied with Their Lives.” Accessed October 18, 2011. https://www41.statcan.ca/2007/70000/ ceb70000_002-eng.htm
—————–. 2008a. Seniors. Accessed September 26, 2011. https://www41.statcan.gc.ca/2008/70000/ceb70000_000-eng.htm
—————–. 2008b. “Study: Chronic Pain in Canadian Seniors.” The Daily, February 21. Accessed September 26, 2011. https://www.statcan.gc.ca/daily-quotidien/080221/ dq080221b-eng.htm
—————–. 2009a. Population Projections for Canada, Provinces and Territories, 2009-2036. Accessed September 26, 2011. https://www.statcan.gc.ca/pub/91-520-x/91-520-x201
0001-eng.pdf
—————–. 2009b. Statistics Canada Census of Population. Cat. no. 97-563-XCB2006005. Ottawa: Statistics Canada.
—————–. 2010a. Perceived Mental Health. Accessed September 26, 2011. https://www.statcan.gc.ca/pub/82-229-x/2009001/status/pmh-eng.htm
—————–. 2010b. “Study: Projections of the Diversity of the Canadian Population.” The Daily (March 9). Accessed September 26, 2011. https://www.statcan.gc.ca/daily-quotidien/100309/dq100309a-eng.htm
—————–. 2011. Health Trends. Cat. no. 82-213-XWE. Ottaawa: Statistics Canda. Accessed September 26, 2011. https://www.statcan.gc.ca/bsolc/olc-cel/olc-cel?catno=82-213-X&lang=eng
Stobert, S., and K. Cranswick. 2004. “Looking after Seniors: Who Does What for Whom?” Canadian Social Trends, Statistics Canada, cat. no. 11-008. Ottawa: Statistics Canada.
Stones, M.J., and L. Stones. 1998. “Ageism: The Quiet Epidemic.” Canadian Journal of Public Health 89 :369-70.
Tarlow, B.J., S.R. Wisniewski, S.H. Belle, M. Rubert, M.G. Ory, and D. Gallagher-Thompson. 2004. “Positive Aspects of Caregiving: Contributions of the REACH Project to the Development of New Measures for Alzheimer’s Caregiving.” Research on Aging 26 (4): 429-53.
United States. 1991. General Accounting Office. Canadian Health Insurance Lessons for the United States. Accessed September 26, 2011. https://archive.gao.gov/d20t9/ 144039.pdf
Van Dalen, H.P., K. Henkens, and J. Schippers. 2009. “Dealing with Older Workers in Europe: A Comparative Survey of Employers’ Attitudes and Actions.” Journal of European Social Policy19: 47-60.
van Kan , G.A., Y. Rolland, M. Houles, S. Gillette-Guyonnet, M. Sota, and B. Vellas. 2010. “The Assessment of Frailty in Older Adults.” Clinics in Geriatric Medicine 26 (2): 275-86.
Vitaliano, P.P., J. Zhang, and J.M. Scanlan. 2003. “Is Caregiving Hazardous to One’s Physical Health? A Meta-analysis.” Psychological Bulletin 129 (6): 946-72.
Vogt, T.M, M. Aickin, F. Ahmed, and M. Schmidt. 2004. “The Prevention Index: Using Technology to Improve Quality Assessment.” Health Services Research 39 (3): 511-30.
Walker, B.L., N.J. Osgood, J.P. Richardson, and P.H. Ephross. 1998. “Staff and Elderly Knowledge and Attitudes toward Elderly Sexuality.” Educational Gerontology 24 (5): 471-89.
Ward-Griffin, C., and V. Marshall. 2003. “Reconceptualizing the Relationship between ‘Public’ and ‘Private’ Eldercare.” Journal of Aging Studies 17: 189-208.
Wenger, C., G. Grant, and M. Nolan. 1996. “Older People as Carers as well as Recipients of Care.” In Sociology of Aging: International Perspectives, edited by V. Minichiello, N. Chappell, H. Kendig, and A. Walker. Australia: ISA Research Committee on Aging.
WHO (see World Health Organization)
Wilkins, K. 2006. “Government-Subsidized Home Care.” Health Reports 17 (4): 39-42.
Williams, A.P., P. Deber, and A. Gildiner. 2001. “From Medicare to Home Care: Globalization, State Retrenchment, and the Profitization of Canada’s Health-care System.” In Unhealthy Times: Political Economy Perspectives on Health and Care in Canada, edited by P. Armstrong, H. Armstrong, and D. Coburn. Toronto: Oxford University Press.
Williams, C. 2005. “The Sandwich Generation.” Canadian Social Trends 77 (Summer): 16-24.
Wister, A.V. 2005. Baby Boomer Health Dynamics: How Are We Aging? Toronto: University of Toronto Press.
Wood, G., A. Wilkinson, and M. Harcourt. 2008. “Age Discrimination and Working Life: Perspectives and Contestations — A Review of the Contemporary Literature.” International Journal of Management Reviews 10 (4): 425-42.
World Health Organization (WHO). 2001. “International Classification of Functioning, Disability and Health (ICF).” Accessed September 27, 2011. https://www3.who.int/icf/ intros/ICF-Eng-Intro.pdf
—————–. 2002. Active Ageing: A Policy Framework. WHO/NMH/NPH/02.8. Accessed September 17, 2011. https://whqlibdoc.who.int/hq/2002/WHO_NMH_NPH_02.8.pdf
—————–. 2007. Global Age-Friendly Cities: A Guide. Geneva: WHO.
This publication was published as part of the Faces of Aging research program under the direction of Sarah Fortin and Nicole Bernier. The manuscript was copy-edited by Barbara Czarnecki, proofreading was by Lori Anderson, editorial coordination was by Francesca Worrall, production was by Chantal Létourneau and art direction was by Schumacher Design.
Neena L. Chappell holds the Canada Research Chair in Social Gerontology and is a professor of sociology in the Centre on Aging at the University of Victoria. She was founding director of the Centre on Aging at the University of Manitoba (1982-92) and the first director of the Centre on Aging at the University of Victoria (1992-2002). Her work in gerontological research focuses on issues around aging (caregiving, social support, dementia care, health serv- ices, healthy aging, Chinese and China) and health and social policy. She has written more than 300 academic arti- cles, chapters, reports, written or edited 9 books, has lectured internationally and is frequently sought out by com- mittees and the media.
To cite this document:
Chappell, Neena L. 2011. Population Aging and the Evolving Care Needs of Older Canadians: An Overview of the Policy Challenges. IRPP Study 21. Montreal: Institute for Research on Public Policy.