
Cette Étude IRPP examine la possibilité d’introduire un mécanisme de capitalisation pour financer les médicaments sur ordonnance pour les personnes âgées en vue d’assurer la viabilité financière du système de santé public. Mark Stabile et Jacqueline Greenblatt préconisent cette solution, tandis que Michel Grignon s’y oppose.
Puisant à des données canadiennes et de l’OCDE, Stabile et Greenblatt prennent d’abord la mesure du défi que représente le financement des soins de santé. Ils montrent que les coûts liés aux soins de santé ont augmenté à un rythme plus rapide que les revenus. De 1982 à ce jour, par exemple, ils ont augmenté en moyenne de 6,9 p. 100 par année, alors que le PIB ne progressait que de 5,7 p. 100. Données à l’appui, les auteurs font également voir que les taux d’imposition moyens ont reculé durant cette période. Ces tendances expliquent que les soins de santé occu- pent aujourd’hui la part du lion des dépenses de programmes des provinces au détriment d’autres secteurs de dépense prioritaires. Ce déséquilibre risque de s’accentuer avec le vieillisse- ment de la population, d’où l’importance pour le Canada d’envisager de nouvelles sources de revenu pour continuer de financer de façon équitable et durable notre système de santé.
À cette fin, les auteurs estiment qu’il faut sérieusement envisager d’introduire un mécanisme de capitalisation pour aider à financer les médicaments pour les personnes âgées de 65 ans et plus. Selon eux, l’augmentation accélérée des dépenses en médicaments et le schéma d’utilisa- tion des médicaments sur ordonnance chez cette clientèle font que ce type de dépense se prête bien à un tel mode de financement. Pour illustrer les coûts de transition, ils présentent, à par- tir de l’exemple du régime de médicaments de l’Ontario, des simulations permettant d’évaluer selon différents scénarios la part du PIB nécessaire au financement du programme sur une pé- riode de 50 ans. Tout en reconnaissant que ce mode de financement comporte des incon- vénients, ils soutiennent que les avantages l’emportent sur les défauts.
Dans son commentaire, Michel Grignon convient qu’une hausse des dépenses en médicaments est inévitable mais affirme que la capitalisation ne réglerait pas le problème de financement que cela soulève. Il examine les trois arguments de fond qui sous-tendent la proposition de Stabile et Greenblatt, et conclut que : 1) la capitalisation n’est pas un moyen efficace de faire face à l’augmentation systémique des dépenses en médicaments ; 2) l’impact financier du vieillisse- ment de la population sur les régimes d’assurance-médicaments sera moins important que ne l’anticipent les auteurs ; et 3) le mécanisme de financement actuel ne créera pas un problème d’équité intergénérationnelle si l’on tient compte des gains de santé découlant de la recherche- développement pharmaceutique. La vraie question soulevée par l’augmentation des dépenses en médicaments sur ordonnance n’est pas tant de savoir si nous pouvons la financer ni à quel moment, mais bien d’établir s’il est politiquement possible de continuer à le faire au moyen de l’impôt sur le revenu.
The aging population will inevitably change the context in which the welfare state operates in Canada and around the world. The specific impacts of this phenomenon on program and service delivery and on financing are, however, up for debate. Yet even though uncertainty surrounds the effects of the aging population, an analysis of Canada’s current health care system through the lens of elder care points to a major challenge in social policy: a rise in the costs of health care. The fiscal parameters of social policy are increasingly being defined by the growing share of health care spending in public budgets; projections assume that this trend will be mildly exacerbated by population aging, even without enhancements to address existing gaps in coverage. Meanwhile, other areas of social policy, such as education, child development and income security, remain inadequately addressed. Responding to these challenges will require a renegotiation of the implicit intergenerational contract that underpins Canadian social policy.
The existing intergenerational contract could be summarized as follows: The current working generation supports the benefits of retirees in order to respect and reward the contribution made by these retirees over their working lives; the current design of the retirement and health benefits system rests on the assumption that this arrangement will remain intact for future generations. A new contract might run along the following lines: Instead of expecting future generations to support their retirement and health benefits, those who benefit from the social infrastructure and economic prosperity over their lifetimes will invest for their own future needs. A new design of the retirement and health benefits system would therefore have to be integrated into a broader set of social policies; this new system should honour past commitments, but may not include the same benefits for future generations.1 When renegotiating this implicit contract, we would need to reevaluate how we deliver care to the elderly population as well as how we finance it. In this paper, we propose a new way of financing the increased costs of health care, particularly those associated with elderly Canadians.
We first review the extent of the policy challenge of providing care to the elderly in the context of population aging, drawing on Canadian and OECD data. We argue that the increase in public health care spending has outpaced the increase in revenues, and that as a result provincial budgets are skewed toward these costs, to the detriment of other spending areas. We realize that this problem is not unique to Canada. Indeed, the majority of OECD countries have seen health care costs rise more rapidly than revenues over the past several decades, and these countries are all considering options that will allow them to continue financing care in an equitable and sustainable fashion.
We then propose a shift from our current pay-as-you-go (PAYGO) model, to a prefunding model for pharmacare for older Canadians. A prefunding insurance scheme in which taxpayers pay into a dedicated fund during their working years to cover health care in their retirement years would ensure continued public funding of our system, while addressing its current inadequacies.
We realize that improvements to the efficiency of health care delivery – increases in the value we receive for the money we spend – are an important aspect of the evolution of our health care system. However, we argue that the experience of other OECD countries and of the Canadian provinces suggests that increasing value for money will not be sufficient to cover all health care expenditures. Therefore, a discussion of policy options for increasing revenues is warranted.
Canada’s current mechanism for financing health care does not provide the revenues required to match expenditure growth. In this section we show that health care costs have risen at rates faster than those for economic growth, and that they will continue to do so. We present some national evidence indicating that tax rates have also been on the decline. The evidence suggests that, in most provinces, this has resulted in a larger share of the provincial budget being dedicated to health care, at the expense of other budget items, including many social programs that contribute to population health.
In the past few decades, OECD countries have experienced increases in health care spending in excess of economic growth. Hagist and Kotlikoff (2005) present the annual growth rates of real government health care expenditures between 1970 and 2002 for 10 OECD countries, all of which fall between 3.91 and 6.23 percent, averaging at 4.89 percent. The authors provide real GDP growth rates for these 10 countries in the same period, which average 2.87 percent. The ratio of health care expenditure growth rate to GDP growth rate runs from 1.32 (for Canada) to 2.01, averaging at 1.70 (Hagist and Kotlikoff 2005). Furthermore, health care spending increased as a share of total public spending between 1995 and 2000 in all OECD countries for which data are available for the period (Flood, Stabile, and Tuohy 2009).
Hagist and Kotlikoff (2005) further break down expenditure growth into the share accounted for by demographic change and that resulting from changes in benefit levels – that is, “health expenditures per person at a given age” (1). The authors find that although demographics play a role in the increase in health care expenditure, the effect of growth in benefit levels “is primarily responsible for overall growth in expenditures per capita” (9). They find that the largest driver in this increased benefit is technological change. Though the authors point out that Canada has had comparatively modest benefit growth, they remind us that, at an annualized rate of 2.32 percent (9), “since healthcare benefit levels are much higher for the elderly than they are for the young, continuing to let benefit levels grow as a country ages will accelerate the increase in healthcare spending” (2). Canada is by no means the only country whose growth rates in health care expenditure exceed its economic growth rates, but the increasing weight of health care expenditure within provincial budgets risks crowding out other government spending areas.
The aging of the baby boomer cohort may loom large in our minds with respect to the pressures that this demographic phenomenon may place on our health care system. Yet health care financing in Canada is in a precarious situation now, because of past trends, rather than being threatened in the future because of an aging population.
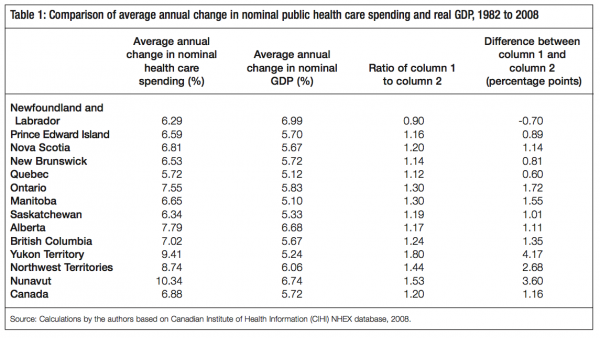
The first of these past trends is growth in government health care expenditure vis-à-vis growth in the economy. Table 1 depicts the average annual growth in nominal government health care expenditure between 1982 and 2008. Ontario’s spending, for instance, grew annually by 7.55 percent, while Alberta’s and British Columbia’s grew by 7.79 and 7.02 percent, respectively. Quebec’s health care expenditure grew by 5.72 percent – the lowest average annual growth of all the provinces and territories. Nominal GDP, however, grew less than these expenditures between 1982 and 2008 in all the provinces and territories except Newfoundland and Labrador. In Ontario, for instance, GDP grew by 5.83 percent annually, on average, while in Alberta and British Columbia it grew by 6.68 and 5.67 percent, respectively. In Quebec it grew by 5.12 percent. Except for Newfoundland and Labrador, the ratio of health care expenditure growth to GDP growth is always greater than 1, meaning that growth in health care spending has increased faster than growth in GDP. In Ontario, Alberta, British Columbia, Manitoba, Saskatchewan and Nova Scotia, the difference between the annual growth rate of government health care expenditure and the annual growth rate of GDP is greater than one percentage point. It is worth noting that the growth in health care expenditure described in table 1 is limited to public spending; it does not include any increases or growth in expenditures on health care in the private sector, either through private insurance or out-of-pocket payments made by individuals.
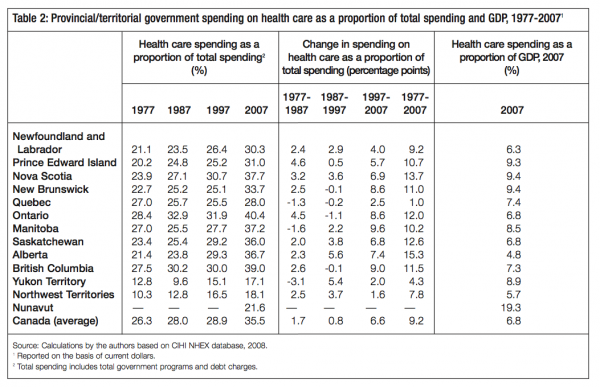
Because health care spending growth rates have outstripped those of the GDP, and because tax rates have been lowered in many provinces, health care has been consuming an increasing share of provincial revenues and expenditures, often crowding out other areas of spending.2 Table 2 illustrates the effects of this growth in health care expenditure by showing health care expenditure as a proportion of total government expenditure (including spending on programs and the debt). In 1977 the provinces allocated between 20.2 percent (Prince Edward Island) and 28.4 percent (Ontario) of their budgets to health care. By 1987 the share of health spending had shifted upward, to between 23.5 percent (Newfoundland and Labrador) and 32.9 percent (Ontario). Again, in the period 1987 to 1997 it shifted slightly upward, to between 25.1 percent (New Brunswick) and 31.9 percent (Ontario). And from 1997 to 2007 it shifted dramatically upward, to between 28 percent (Quebec) and 40.4 percent (Ontario).
From 1977 to 1997 there were both negative and positive changes to the health care portion of the total budget across the provinces, but from 1997 to 2007 all provinces and territories increased the health care share of their budget by an average of 6.6 percentage points. And from 1977 to 2007 eight provinces increased it by more than 10 percentage points. Quebec is the only outlier in this regard, as it increased its share on health care spending over the three decades by only one percentage point (in fact, it even reduced it between 1977 and 1997).
Projections over the medium term suggest that the share of public spending devoted to health care is likely to continue to increase. We focus here on Ontario, drawing on projections from Towards 2025: Assessing Ontario’s Long-Term Outlook (Ontario Ministry of Finance 2005), although many provinces are likely facing similar projections. The report assumes a 2.2 percent annual increase in government health care spending based on the combined effect of population growth and aging. It further assumes that health care spending will also increase by 2.2 percent annually due to price inflation. Finally, increases in utilization rates will lead to another 1.5 percent annual increase. The province thus estimates that, overall, government health care expenses will rise 6 percent annually over the next 20 years. The authors of the report believe that, based on these assumptions, “the share of health spending in total program spending [excluding any spending on the debt] would climb from 45 percent in 20042005 to about 55 percent in 2024-2025” (95), thus leaving 45 percent of the government’s budget for all other programs and service, absent any changes in tax policy.
In the previous section we saw that, for the past few decades, health care costs have grown at rates exceeding those for the economy. In addition, many OECD countries have responded to increased global competition and mobility by lowering their tax rates over the past several years, leading to a reduction in the availability of public funds. Across OECD nations, tax revenue as a percentage of GDP increased, on average, from 30.3 percent in 1975 to 37.1 percent in 2000, but dropped to 36.3 percent in 2003 (Flood, Stabile, and Tuohy 2009). This pattern holds for the majority of OECD countries for which data are available. For instance, in Canada total tax revenue as a percentage of GDP was 31.9 in 1975, grew to a high of 35.9 in 1990 and remained steady at 35.6 until 2000, but then fell to 33.8 in 2003.
Such policy choices have contributed to the financing crunch. While simply increasing general tax rates would be one policy option for addressing rising health care costs, the fact that these costs have exceeded GDP growth, and the apparent reluctance of OECD countries to raise general taxes, suggest that it may be prudent to consider alternative sources of funding. Such a policy move, together with the strenuous efforts being made in many jurisdictions to contain the rise in health care costs, may free up more revenues to meet the funding needs of the health care system.
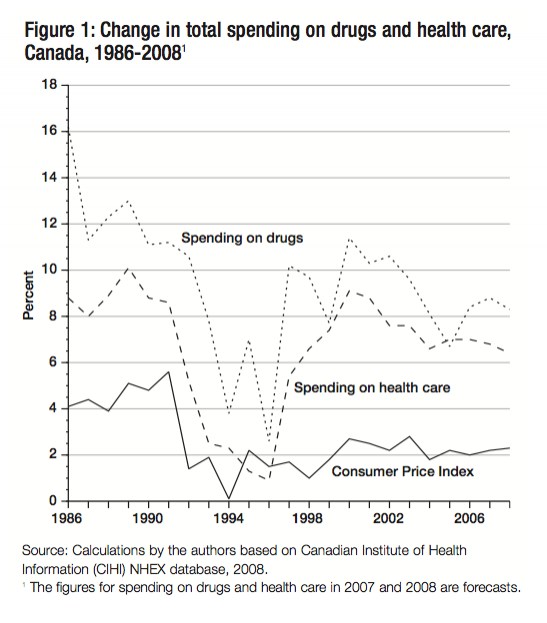
There are several reasons why any discussion of financing health care costs, particularly those associated with the elderly population, must consider prescription drug costs. First, prescription drugs are among the fastest-growing components of health care spending in Canada. Figure 1 shows the yearly growth rate for health services in general and pharmaceuticals in particular. Every year from 1986 to 2007, the growth rate of expenditures on prescription drugs has exceeded the overall growth rate for health care spending, and in many years, it has been double-digit.
Second, while health care expenditures in general tend to be concentrated among a few very sick individuals, pharmaceutical expenditures are much more evenly distributed among the population. This is particularly true for the population aged 65 and over.
Morgan (2006) examines prescription drug use in British Columbia between 1996 and 2002. He finds that by the age of 60 approximately 80 percent of men and 90 percent of women are using at least one prescription drug, and that by the age of 70 some 85 percent of men and 95 percent of women are using at least one prescription drug. Not only does the probability of pharmaceutical use increases with age, but the number of different drugs used also increases with age. Among 40-year-old prescription drug users, the average number of different drugs used is between 2 and 2.5, while among those aged 80 and over the number rises to more than 4 (Morgan 2006). Increased prescription drug use by an aging population is compounding and overall increase in drug use. When a critical mass of baby boomers reaches the age of 65, thus becoming entitled to pharmacare benefits (as per their province’s age-related drug program), provinces will face increasing costs in the provision of drug benefits (Morgan 2008, 209).
In addition to the almost universal use of several prescription drugs by the elderly, the distribution of use is relatively uniform. Morgan (2008) shows that among those 65 and over in British Columbia, less than 40 percent of drug expenditures are attributed to the top 10 percent of users. This is significantly different from the use of health services more generally. Forget, Deber, and Roos (2002) demonstrate that among those 65 and over in Manitoba, 75 percent of physician and hospital expenditures are incurred by the top 10 percent of users. While there may be modest differences in utilization across the provinces, it appears that, compared with pharmaceutical utilization, general health care utilization is far more skewed toward the sickest.
The conclusions to be drawn from these findings are that the elderly are extremely likely to need pharmaceuticals both now and in the future, and the need for pharmaceuticals is more evenly distributed across the elderly population than the need for health services more generally.
A third reason to consider pharmaceuticals specifically is that, in Canada, access to prescription drug insurance is far less universal than access to insurance for other forms of health care. This incomplete coverage has a greater impact on the elderly than on other age groups. Prescription drugs used outside hospitals are not considered “medically necessary” under the Canada Health Act, and therefore are not automatically included in publicly funded provincial insurance schemes. As a result, coverage of prescription drugs has not evolved uniformly across the provinces and territories, and many Canadians find themselves either uninsured or underinsured. A 1997 report by Health Canada notes that “the overall trend produced by public sector reaction to increasing drug costs has been toward changing public coverage for drugs based on one’s ability-to-pay. The report goes on to explain that “this approach has reduced the rate of increase of public sector drug expenditure” (20). In order to reduce the rate of increase, provinces changed their drug plans in the 1980s and early 1990s by employing formularies or lists of drugs eligible for reimbursement; using reimbursement ceilings and reference-based pricing to limit the amount paid for drugs; negotiating or limiting pharmacy dispensing fees and encouraging the dispensing of larger quantities to minimize these fees; restricting the eligible population; and imposing or increasing payments made by individuals (such as co-payments and deductibles).
Ontario, Alberta and the Atlantic provinces offer drug plans to the elderly and to social assistance recipients. British Columbia, Manitoba and Saskatchewan now offer plans to those whose drug costs exceed income-based deductibles (regardless of the individual’s age). Quebec, on the other hand, requires that all residents purchase premium-based drug insurance, either through their employer (if the employer offers it) or through the government (Morgan 2008). There is thus no universal drug plan across the provinces and territories, and one might wonder how this variation in drug insurance plans fits with the concept of “portability” in the Canada Health Act.
A tangent to the question of equal access across jurisdictions is that of public versus private costs. A study by Willison, Grootendorst, and Hurley (1998) simulated the costs incurred by a typical elderly person, with a given profile of province of residence, marital status, income, and drug consumption. Two findings stand out. First, the elderly faced a substantial burden in out-of-pocket costs associated with the average prescription drug pattern, and there was an almost tenfold difference in the out-of-pocket payments for the same consumption of drugs for individuals, with similar income levels, among the 10 provinces. For example, the authors report that among those who received the federal Guaranteed Income Supplement, out-of-pocket costs for the average expenditure scenario on a basket of prescription drugs varied from $45 in Ontario to $450 in Saskatchewan (11). Second, irrespective of province of residence, most elderly people faced an increasing cost for the same basket of drugs in the period between 1990 and 1997. Health care costs are straining not only the public purse but also the private purses of Canadians.
These gaps in coverage will continue to widen as pharmacare becomes an increasingly large share of health care. Pharmaceuticals make up a larger share of our health care package now than they have ever before. While inflation-adjusted expenditure per capita on hospital care increased by 51 percent (or 1.4 percent per year) from 1975 to 2006, it increased by 98 percent (or 2.2 percent per year) for physician services and by 338 percent (or 4.9 percent per year) for pharmaceuticals (Morgan 2008). More concretely, in 1995 the average number of physician visits per individual was four per year, while the average number of prescriptions filled by individuals was almost eight (Stabile 2001). Though pharmacare may replace some health services (for instance, a person might receive pharmaceutical treatment instead of surgery), potential expenditures in this field are almost limitless – there is always a demand for more and better care. Technological advances also tend to increase demand and costs rather than allow for costsaving substitutions of one form of care for another (Gunderson and Hyatt 2008).
W e propose prefunding certain aspects of health care for the elderly as one part of the solution regarding more sustainable health care financing. Prefunding in this context implies that individuals pay into a fund during their working lives in order to cover expenditures that are highly likely to occur.
Pre-funding is currently used to partially fund the Canada and Quebec old-age pension plans (CPP-QPP).3 The CPP-QPP model functions well for many reasons. For example, it ensures that the elderly have part of the income they need in order to cover a wide range of predictable expenditures. Peoples’ health care needs, however, are somewhat uncertain. Nonetheless, as we have shown above, certain areas of health care expenditures occur among the elderly with more certainty and are more evenly distributed than others, thus more closely mimicking the need for a savings function provided by income replacement plans. Pharmacare for the elderly appears to be a prime candidate for prefunding since, at the cohort level, the pharmaceutical needs of this segment of the population are relatively predictable.
In the remainder of this paper we describe a model for prefunding prescription drugs for the elderly inspired by the success of the CPP-QPP model and provide some preliminary estimates of the costs of such a model. We propose that medically necessary services that are currently funded through a variety of tax measures in most provinces remain so, but that, over time, the majority of prescription drug funding come from prefunding rather than from the tax pool and out-of-pocket spending.
Prefunding for health services more broadly has been studied in Canada. At least two reports have made cases for prefunding that are consistent with the arguments presented here. The first, the Clair Commission in Quebec, proposed prefunding for part of Quebec’s health care costs. In explaining its rationale, the commission used many of the same justifications discussed above, including those of intergenerational equity and sustainable funding (Commission d’étude sur les services de santé et les services sociaux 2001).
Robson has also argued convincingly for prefunding part of health care (2002). He too cites intergenerational equity, as well as the higher costs expected through demographic changes, as driving the need for additional revenues to cover public health care. He provides preliminary estimates of the costs of prefunding for three sets of health care costs: a partially prefunded health grant for the elderly, partial prefunding of the entire health budget in Alberta, and partial prefunding of the Ontario Drug Benefit.
Here we focus on updating the proposal to prefund the Ontario Drug Benefit, as prescription drug spending represents the strongest case for prefunding. Ontario is presented as a test case for what might be conceived of as a national program.
Prefunding has been explored in other jurisdictions as well. For example, Fuchs (1998) offers prefunding of Medicare (the insurance program for the elderly in the United States) as a potential solution to rapid increases in the cost of coverage. Fuchs also suggests that additional revenue sources be explored together with options for slowing the growth of government health care spending.
A model for prefunding a program such as the Ontario Drug Benefit calls for individuals to pay a premium while they are in the workforce in order to partially prefund drug coverage once they reach a certain age. We believe that the most efficient way for an individual to contribute is through a payroll deduction. The program could be designed so that employers are required to contribute as well. Contributions would almost certainly be scaled to income, and could be capped. For instance, as of 2009, CPP-QPP contributions are capped at approximately $46,300. (Note that the lower the cap on contributions, the greater the share of the burden carried by lower-income individuals relative to their income.) However, our model differs from the CPP-QPP in at least two ways.
One difference is the prefunding model serves a partial insurance function, where risks are pooled across the cohort; it is thus not an “individual” savings account. As we have seen, prescription drug use is distributed much more evenly across an age cohort than is the case with other forms of health care use, but in our model those individuals who require fewer drugs would be cross-subsidizing those who require more. Coverage would be dictated by health needs, not by contributions paid.
Also, since the prefunding model would not link benefits solely to the contributions paid, the level of redistribution would be such that individuals with higher incomes would pay more into the fund than those with lower incomes, up to a ceiling, if we choose to have one. The degree of risk-sharing and redistribution would need to be determined. The prefunding model allows for many different combinations. We suspect, however, that Canadians would want this plan to share the values reflected in the rest of the Canadian health care system.
In addition to allowing risk-sharing and redistribution, there are several other benefits to this method of prefunding. First and foremost, it sets aside savings today for expenditures that are clearly anticipated and threaten to put considerable pressure on public budgets. If left unaddressed, these expenditures could lead to the crowding out of other social services within provincial budgets, more deficit financing, further privatization of the health care system, or a higher tax burden on the working-age population of the day.
Second, prefunding through a payroll-deduction system would build on an extensive framework of employment-based insurance payments for health services not covered by the Canada Health Act. Approximately two-thirds of working Canadians receive health care benefits through their employer (Stabile 2001), and many cost-share these benefits through payroll contributions. Third, the prefunding model leaves in place the current funding mechanisms for services covered by the Canada Health Act, thus avoiding debate about the public-private mix of health services. Fourth, it freezes a part of the fastest-growing portion of provincial health care budgets – prescription drug benefits, primarily for the elderly – and could free up resources for other priorities. Finally, as the Clair Commission noted (Commission d’étude sur les services de santé et les services sociaux 2001), prefunding provides some assurance to the current generation that they will not be saddled with growing health care costs for the generation that preceded them.
While in theory such a prefunding program could be either mandatory or voluntary, we propose a mandatory program. A system of mandatory contributions would ensure that individuals are able to afford their drug expenses when they reach old age and would address the problem of healthy people opting out of the program, which undermines both cost-sharing and risk-sharing.
There are some potential drawbacks to prefunding that are worth noting. The funding payment, resembling a payroll tax in its simplest form, could negatively affect employment and might not be the most economically efficient way to raise tax revenues (Gunderson and Hyatt 2008). However, the extent to which any payroll deduction that is tied to a specific benefit affects employment will depend on the extent to which workers value the resulting benefit (Summers 1989). If, from the perspective of the payer, the deduction approximates the value of the benefit, then the payer will be prepared to accept the benefit in lieu of income and the unemployment effects will be minimal. In this respect, a prefunded benefit differs from the general tax used to fund social services – it is earmarked for a particular benefit and the rates are linked to the costs of that benefit, so that the payers of the tax can see the value of the benefit.
Also, there are currently many insurers that cover retirement benefits, including prescription drugs for the elderly. The interactions between private insurance and a prefunded drug benefit could be complex. Issues such as which would be the primary and which the secondary payer will have to be worked out, and care would have to be taken to avoid undermining the existing insurance market. However, these issues, while complex, are not insurmountable. In provinces where public pharmacare programs already exist, some of these have been sorted out.
There are also questions of federal-provincial jurisdiction that will necessarily complicate any effort to institute a national drug benefit. While the CPP-QPP infrastructure might appear to be an efficient mechanism for implementing a prefunded drug benefit, this would require federal-provincial cooperation, and a willingness on the part of the federal government to oversee a major social program. It is therefore more likely that an initiative of this sort would be launched at the provincial level, possibly modelled on the CPP-QPP.
Another potentially negative aspect is that, viewed strictly from the perspective of progressivity, a payer system is a more regressive form of taxation than general income taxes. However, as Glied (2008) points out, another dollar spent on health care may be less progressive than a dollar spent on social assistance or public education. This is because rates of health care utilization are higher among the elderly and, among the elderly, those of higher socio-economic status tend to live longer and therefore to use more health care. Conversely, social assistance is generally focused on individuals of low socio-economic status. Not to discount the importance of progressivity, but to insist that each additional tax dollar be as progressively raised as the last, is to ignore a broader progressive agenda in government spending. Thus in our view there is no reason not to explore, from an equity perspective, the potential for a larger role for prefunding in the health care system, particularly if this allows for the spending of tax dollars on other, equally critical public programs.
Finally, there are many design questions that would need to be considered and that might be resolved in multiple ways. These include the establishment of a formulary (whether provincial or federal); the management of the fund (whether private or public); the use of deductibles and co-payments; the progressivity and scope of the pre-payments; and integration of a pharmacare program into existing employer plans.
We use the Ontario Drug Benefit (ODB) program as an example of a prescription drug benefit that could be covered through prefunding. This exercise is meant simply to illustrate the costs of prefunding a major drug program, not to suggest the various policy parameters that should be chosen; we leave that exercise for future work.
The ODB covers prescription drugs for Ontarians aged 65 and over, as well as residents of long-term care homes and homes for special care, recipients of professional home services and social assistance, and recipients of the Trillium Drug Program. It manages a formulary and its coverage includes deductibles and co-payments. In 2008-09 the Ontario government projected it would spend $3.6 billion on the ODB and expected these costs to grow by 6.9 percent, slightly higher than the average growth rate of 6.2 percent in the overall health care budget. The ODB currently accounts for approximately 9 percent of all health care spending by the Ontario Ministry of Health and Long-Term Care (Ontario Ministry of Finance 2009).
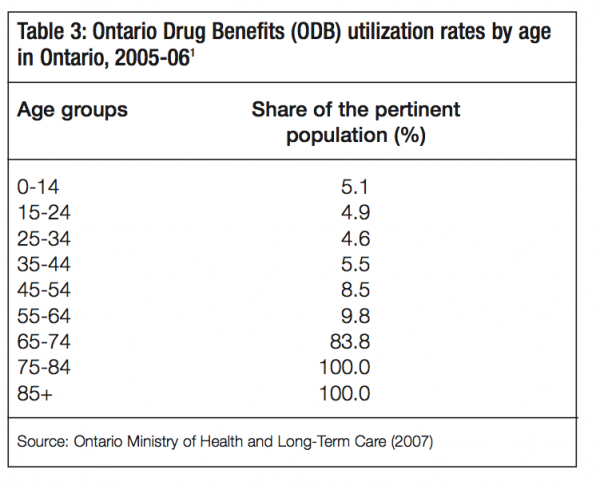
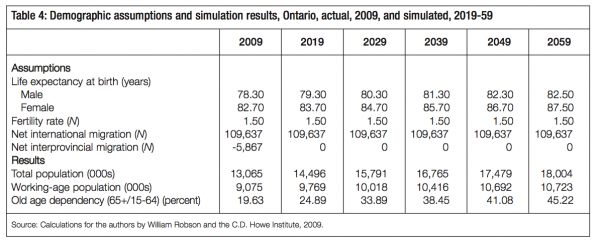
We update and modify the prefunding projection model used by Robson (2002) to simulate the costs of prefunding the ODB over the long run.4 We use the 2005-06 ODB utilization rates by age from data provided by the Ontario Ministry of Health and Long-Term Care (2007) to estimate per-person government spending in each age group (table 3). Our assumptions regarding life expectancy, fertility and migration are presented in table 4.
We model spending assuming three levels of spending growth – 4, 6 and 8 percent. Over the past several years, spending growth in the ODB has exceeded 6 percent and has often been close to 8 percent, so we view these assumptions as realistic. As in Robson (2002), we assume real GDP growth of 1.8 percent annually per person aged 15 to 64. Finally, we model two potential returns on fund assets, 3 percent and 5 percent. Using these scenarios, we model the share of GDP required to fund the ODB over a 50-year time horizon.
It should be apparent that with an assumed real economic growth of 1.8 percent and growth in the ODB of between 4 and 8 percent, the share of GDP required to fund the ODB will automatically increase. Assuming a 4 percent growth in ODB costs, the share of Ontario’s GDP required to fund the ODB would rise from the current 0.62 percent to 1.3 percent in 50 years’ time. Using the more historically consistent rate of 8 percent growth in spending, the share would rise to a startling 8.6 percent of GDP. This modelling assumes that the current ODB policy parameters remain unchanged (captured in the current utilization rates by age), including co-payments and deductibles.
The results of the simulation are presented in table 5. We show the amounts required to stabilize the ODB in the long run based on the three cost-growth and two asset-growth scenarios noted above. The first column shows the value of the fund (in 2009 dollars). The second shows the contribution to the fund as a share of GDP. We present two per-person estimates – a gross contribution amount required to stabilize the entire ODB fund (third column) and a net contribution amount, defined as the amount required to fund the difference between total future ODB spending and current ODB spending (fourth column). The net contribution assumes that the government will continue to fund the ODB at current levels but will not cover any incremental costs going forward.
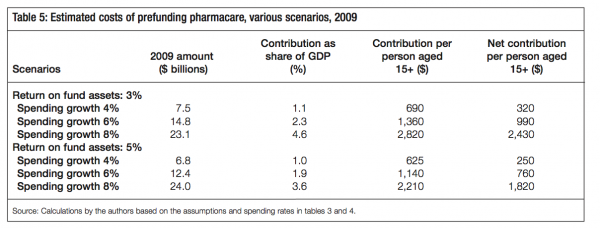
Two points are worth noting here. First, these are large amounts – net annual contributions range from $320 per person aged 15 to 65 to as high as $1,820 in the high-cost growth scenario. These amounts are to be expected in order to stabilize spending, which in most cases grows faster than both the economy and the fund being used to stabilize it. Nevertheless, if growth in drug costs is lower than the rates assumed here, or if economic growth is higher, the prefunding payment amounts would fall. It is worth reiterating that the high costs are generated by the historical growth rate in prescription drug spending and are not a function of choosing to cover these through prefunding.
Second, these amounts represent averages across the population and are not the amounts that all individuals would be required to pay into the fund. It is extremely unlikely (undesirable, in fact) that a prefunded benefit would be implemented in this way. The likely scenario would be a distribution of payment levels based on income, either proportionally or progressively over some income range, leaving some paying much less and others much more. Further simulations are needed to determine the fairest and most efficient way of structuring the premiums. Cutler et al. (1990) and Auerbach, Gokhale, and Kotlikoff (1994) provide some of the foundations for such analyses in their explorations of the efficiencies and fairness of prefunding mechanisms.
Indeed, many implementation details would need to be worked out, including transition issues, cost-sharing arrangements between employers and employees, eligibility restrictions, and primary versus secondary payer restrictions. Our aim in this study is simply to underline the prudence of considering a prefunding arrangement for the fastest-growing portion of our health care spending now, while there is still time to address the future need for financing.
In Canada, health care costs are rising at rates that exceed the growth in our economy. These increasing costs, coupled with policy choices to reduce general tax rates, have led to a larger share of provincial budgets going to health care.
This is true across the country, as well as in many of the OECD countries for which data are available. Canada is not unique in experiencing difficulty sustaining the increasing cost of funding health care.
We propose that health care funding be stabilized through the prefunding of the component of health care whose costs have grown particularly rapidly – prescription drugs for the elderly. Not only has the growth rate in prescription drug costs exceeded the overall growth rate in the cost of health services, but the elderly use a much larger share of prescription drugs than do the general population. In addition, the distribution of health care among the elderly has been shown to be even more for prescription drugs than for health services in general. Some funding mechanism will thus be required to help cover these costs, which almost all elderly Canadians face.
Our proposal builds on Canada’s success in prefunding parts of our income replacement programs through the Canada and Quebec pension plans. We therefore propose that individuals pay into a fund during their working lives to provide a prescription drug benefit for their retirement years. While our preliminary estimates of the cost of prefunding pharmaceuticals suggest that Canadians will need to pay considerably more for their health care, our model helps to make transparent the cost of paying for ever-growing health care needs and the benefits of starting to cover these costs early on. Pre-funding is not without its drawbacks, including transition issues and the difficult design choices required to ensure efficiency and fairness. However, we believe the plan proposed here would help to stabilize the public funding of health care, as well as to restore intergenerational equity in the funding of social benefits and to manage the demographic challenges presented by an aging population.
Auerbach, A., J. Gokhale, and L. Kotlikoff. 1994. “Generational Accounting: A Meaningful Way to Evaluate Fiscal Policy.” Journal of Economic Perspectives 8 (1): 73-94.
Commission d’étude sur les services de santé et les services soci- aux, 2001. Emerging Solutions. Government of Quebec. Accessed February 1, 2010. https://publications.msss.gouv.qc.ca/acrobat/f/documentation/2001/01-109-01a.pdf
Cutler, D., J. Poterba, L. Sheiner, and L. Summers. 1990. “An Aging Society: Opportunity or Challenge?” Brookings Papers on Economic Activity 121 (1): 1-74.
Flood, C. M., M. Stabile, and C. Hughes Tuohy. 2009. “Sustainability, Quality, and Accessibility in the Health Care System.” Unpublished.
Forget, . L., R. Deber, and L. L. Roos. 2002. “Medical Savings Accounts: Will They Reduce Costs?” Canadian Medical Association Journal 167 (2): 143-47.
Fuchs, V.R. 1998. “Health Care for the Elderly: How Much? Who Will Pay for It?” NBER Working Paper 6755 (October). Cambridge, MA: National Bureau of Economic Research.
Glied, S. 2008. “Health Care Financing, Efficiency and Equity.” In Exploring Social Insurance: Can a Dose of Europe Cure Canadian Health Care Finance? edited by C. Flood, M. Stabile, and C. H. Tuohy. Montreal and Kingston: School of Policy Studies, Queen’s University (37-58).
Gunderson, M., and D. Hyatt. 2008. “Payroll-Tax Financed Health Insurance: A Way for the Future?” In Exploring Social Insurance: Can a Dose of Europe Cure Canadian Health Care Finance? edited by C. Flood, M. Stabile, and H. Tuohy. Montreal and Kingston: School of Policy Studies, Queen’s University (91-113).
Hagist, C., and L. J. Kotlikoff. 2005. “Who’s Going Broke? Comparing Healthcare Costs in Ten OECD Countries.” NBER Working Paper 11833. Cambridge, MA: National Bureau of Economic Research.
Health Canada. 1997. Drug Costs in Canada. Report submitted to the Standing Committee on Industry. Ottawa: Health Canada.
Morgan, S. G. 2006. “Prescription Drug Expenditures and Population Demographics.” Health Services Research 41 (2): 411-28.
——————. 2008. “Challenges and Changes in Pharmacare: Could Social Insurance Be the Answer?” In Exploring Social Insurance: Can a Dose of Europe Cure Canadian Health Care Finance? edited by C. Flood, M. Stabile, and C. H. Tuohy. Montreal and Kingston: School of Policy Studies, Queen’s University (199-219).
Office of the Chief Actuary. 2007. “Actuarial Report (23rd) on the Canada Pension Plan as at 31 December 2006.” Ottawa: Office of the Superintendent of Financial Institutions Canada.
Ontario Ministry of Finance. 2005. Towards 2025: Assessing Ontario’s Long-Term Outlook. Toronto: Ontario Ministry of Finance. Accessed February 1, 2010. https://www.fin.gov.on.ca/en/economy/ltr/2005/05_ltr.pdf.
——————. 2009. 2009-2010 Ontario Budget. Toronto: Ontario Ministry of Finance. Accessed February 1, 2010. https://www.fin.gov.on.ca/en/budget/ontariobudgets/2009/papers_all.html
Ontario Ministry of Health and Long-Term Care. 2007. 2005-06 Report Card for the Ontario Drug Benefit Program. Toronto: Ontario Ministry of Health and Long-Term Care. Accessed February 1, 2010. https://www.health.gov.on.ca/english/ public/pub/ministry_reports/odb_report05/odb_rep_05_06.pdf.
Robson, W. B.P. 2002. “Saving for Health: Pre-funding Health Care for and Older Canada.” The Health Papers. Toronto: C.D. Howe Institute. Accessed February 1, 2010. https://www.cdhowe.org/pdf/commentary_170.pdf
Stabile, M. 2001. “Private Insurance Subsidies and Public Health Care Markets: Evidence from Canada.” Canadian Journal of Economics 34 (4): 921-42.
Summers, L. 1989. “Some Simple Economics of Mandated Benefits.” American Economic Review 79 (2): 177-83.
Willison, D., P. Grootendorst, and J. Hurley. 1998. “Variations in Pharmacare Coverage across Canada.” Working Paper 9808. Hamilton: McMaster University Centre for Health Economics and Policy Analysis.
In Ontario, those aged 65 and older and welfare recipients have their prescription drugs covered by a public program, the Ontario Drug Benefit (ODB). The program is funded through taxes, which means that current expenditures are paid from current revenues (as in a pay-asyou-go [PAYGO]) scheme). Stabile and Greenblatt recommend moving toward a form of prefunding whereby a portion of current tax revenues is set aside in an earmarked fund to be used on future prescription drug expenditures for seniors.
Stabile and Greenblatt offer three rationales for prefunding pharmacare:
1. The PAYGO mechanism is not an efficient way of collecting revenues for a health service that is predictable. A compelling argument for PAYGO funding of health care is the efficiency of pooling insurance mechanisms. Since hospitalization is a rare and costly event, it makes perfect sense to spread the risk across as large a population as possible. The authors claim that prescription drug consumption is not a rare and costly event but rather is age-related, and that pharmacare therefore has more in common with the old age pension than with standard health care and, as with retirement pensions, is suitable for prefunding.
2. The PAYGO mechanism is not robust to population shocks. Because of population aging, it will, in the future, generate “too high” a level of taxation for society as a whole (again, similar to retirement pensions). Prefunding would help to smooth this increase in the tax rate.
3. The PAYGO mechanism is unfair. Generations born during low-fertility periods end up supporting a high level of contribution per capita, through no fault of their own. (Ironically, the generation responsible for their high contribution rate is the very one they are supporting.)
Let me make it clear from the outset that although I do not share the authors’ arguments for prefunding pharmacare, I see their paper as an innovative, thought-provoking and insightful treatment of a topic that lies at the core of Canadian health policy concerns for the near future. But despite its merits, I have several reservations and my commentary focuses on the three issues described above.
There are two sources of variability in health care spending. The first is the fact that the amount of health care one needs can vary across individuals around the mean at a given point in time. Let us call it the random component of variability, even though it can be partially determined by observable factors such as age and education. It states that even though we know how much will be spent on health care overall for a given year, we do not know which particular individuals will benefit from it. The other source of variability is the change over time in the population mean of expenditures. Let us call this the systemic component of variability, which states that, for all individuals, health care will be more costly tomorrow than it is today.
From a theoretical point of view, efficiency requires that the former be covered through social insurance (i.e., a PAYGO scheme), to reduce individual uncertainty, and that the latter be covered through savings (i.e., prefunding), to minimize undue or inefficient transfers to the preceding generation. For instance, Fuchs (1998) suggests separating the two sources of variability in health care to address the foreseen increase in spending in the US Medicare scheme: Prefunding would be introduced to cover any future increase in spending above and beyond the current level. This, it must be noted, includes the effect of not only population aging but all other sources of spending increase, such as medical progress and inflation.
This is what Stabile and Greenblatt propose regarding prescription drugs for elderly Canadians. However, it is not clear why prescription drugs would be a better candidate for prefunding than any other component of the health care sector – hospitalization, for example. As noted by the authors, the random component is less important in spending on prescription drugs than it is on inpatient care – at any given moment, more individuals consume drugs than are admitted to hospital. Still, as the authors suggest, the difference between the two is a matter of degree, not of nature. As a matter of principle, there could be some prefunding for hospital care as well (the effect of inflation on the cost of a night in hospital is certainly greater than that for most drugs).
My main concern, however, is with the idea that it is more efficient to finance the systemic component through savings than through insurance. This is certainly true when the systemic component is pure consumption: If we consume more of one type of health care toward the end of life because our need for that type of care increases with proximity to death, then it is efficient to pool resources within a cohort; on an individual basis, this covers the risk of needing that type of care too young or of surviving too long in that situation; on a collective basis, it ensures that each cohort pays for its average cost.
This might work well for long-term care (nursing-home care and home care): We can predict that, overall, the need for long-term care will increase with the aging of the population, and it would make sense to prefund some of that increase in a cohort-based fund (pooling at the cohort level would also reduce inequities in access to long-term care, compared with a purely individual form of savings). This is not to say that it would be easy to predict the systemic component of variability in spending on long-term care. Depending on whether compression or expansion holds true for morbidity in the future, and depending on how gender differences in life expectancy, coupled with marital status, evolve in the next 50 years, we might actually see a decrease in the need for long-term care on a per capita basis. But the impact of the aging of baby boomers on aggregate spending on long-term care in Canada is not ambiguous.
Prescription drugs differ from long-term care in one very important respect: There is a strong investment component in pharmaceutical consumption. Patients who take their treatment are not only consuming drugs, they are also investing in their health capital and enhancing their health status for the future. Of course, some treatments are ill-dosed or ill-prescribed and, as a result, detrimental to health; but most treatments help individuals to achieve better health. In this sense, drugs are not that different from primary care (physician visits). For that very reason, in Canada and in many other countries, primary care is included in the universal health care plan; it is financed through a social insurance (or PAYGO) mechanism rather than being prefunded.
Even though primary care use is even less concentrated than prescription drug use (for example, almost 90 percent of Canadians see a general practitioner at least once a year), it would be odd to prefund GP visits. Prefunding is a way to link contribution to consumption. A larger cohort living longer would contribute more than a smaller, less fortunate one if the per capita amount was fixed and not amenable to current decisions – that is, if there was a finite and limited basket of services. However, because patients use primary care to produce health rather than to enjoy themselves, it would not be efficient to limit the amount of primary care they consume today through a prefunding mechanism.
To summarize, I do not think that the existence of a systemic component in spending variability is a sufficient rationale for deciding whether to pool or to prefund a specific type of care. Another important factor is the consumption and investment shares of the type of health care considered.
Another line of thinking developed in the study is that the PAYGO mechanism is not protected against demographic shocks. Here, the issues are the changes in the size of cohorts (rather than the increase in spending due to medical progress and medical inflation, as in the previous point) and the welfare loss from a societal perspective (rather than from the insurer’s perspective only).
It is certainly true that a PAYGO scheme is not protected against demographic shocks1 whereas a prefunded mechanism may be protected, as long as the shocks can be predicted and their magnitude forecast. Since it is indeed the case that demographic changes are anticipated and their financial consequences forecast with reasonable precision, it is clear that prefunding would be better than the current PAYGO scheme at protecting pharmacare against demographic changes. In other words, prefunding is simply a way of smoothing revenue collection over years (or decades). Instead of raising taxes each year after 2010 (and until 2050 at least) in order to accommodate the increase in the number of prescription drug users, the government would collect more revenue than what is strictly needed to cover expenditures now, in order to collect less than needed in the future.
But why would one want to smooth revenue collection? There is nothing intrinsically right in keeping the tax rate constant or intrinsically wrong in modifying it, as long as its variations can be anticipated by taxpayers. The benefit of smoothing is determined on the basis of two factors.
First, smoothing means that the government increases the tax rate (relative to what is required with PAYGO) when the tax rate is low, and decreases the tax rate (still relative to what would be required with PAYGO) when the tax rate is high; if the gain of taxing less than expected at the higher level is greater than the cost of taxing more than expected at the lower level, there is a benefit in smoothing taxation. There are two reasons why the gain of taxing less at the higher level can exceed the cost of taxing more at the lower level: The opportunity cost of taxation might increase with the tax level, or the disutility of taxation for the rich might be that voters’ support for pharmacare decreases rapidly beyond a given level of taxation.
Second, smoothing means taxing more today in order to tax less tomorrow. Two parameters are important here. The relative value of what occurs now compared to what will occur later is called the time discount rate (TDR); this is one of the main objections against smoothing, since the cost is incurred today (say, between 2010 and 2030), and the benefit will accrue tomorrow (say, between 2030 and 2050). In the economic literature/theory, the rational consumer prefers to consume now and pay later. The other parameter is the interest rate. If governments are reasonable enough not to spend the extra revenue collected today on something else, the compounded interest will generate extra revenue in the fund, and smoothing will actually make us richer in the future.
The key figure here is the difference between the interest rate and the TDR. It is certainly not easy to forecast that difference over the next 40 years, but what is clear is that a difference of only one percentage point has dramatic consequences. For example, if we use – as is often the case in cost-efficiency evaluation – a TDR of 5 percent and assume an average real interest rate of 4 percent per year, the present cost of overtaxing by 1 percent of national income, on average, between 2010 and 2030 so as to undertax by the same rate after 2030, will represent a cost of 6.5 points of national income, or approximately $3,000 per Canadian over the next 40 years.
Overall it is hard to tell whether smoothing is beneficial. It all depends on how much we value our current standard of living as opposed to our standard of living in 30 years’ time, relative to how much we can hope will accrue to dollars saved today over the same period. It also hinges on the magnitude of the financial impact of the foreseen demographic shock. What can be reasonably predicted about the impact of population aging on pharmacare spending?
In all likelihood, the impact of aging on pharmacare will not be great. Forecasts of the impact of aging on total health care expenditures in Canada between 2010 and 2050 vary from one to three percentage points of national income (depending on whether the forecast allows for the effect of proximity to death). Currently, pharmacare covers approximately half of our pharmaceutical expenditures, or 10 percent of total health care expenditures, the other half being covered by private insurance and out-of-pocket payments (see the OECD Health Database for 2009). The effect of aging per se2 on taxation for pharmacare is therefore estimated to be a maximum of 0.3 points of national income over 40 years. This means that Canadians should be taxed $140 more in 2050 than in 2010, in order to finance the impact of population aging on pharmacare (if legislation remains the same).
This is a small amount for the level of uncertainty surrounding it. The total amount to be smoothed is $140 per Canadian, but, as calculated above, the effect of a one-point difference between the TDR and the real interest rate on that amount would be approximately $900 (0.3 times 3,000, since the above $3,000 is calculated for a 1 percent tax rate). Do we want to chance losing $900 to smooth $140?
Moreover, the comparison of costs and benefits of smoothing versus PAYGO for pharmacare assumes that if we maintain the status quo (i.e., fund pharmacare through social insurance only), pharmacare will have to withstand the effect of aging on its own. But things work very differently in real life, and we know that all age-related expenditures are pooled together in the government coffers. As Denton and Spencer (2000) show, population aging will have a neutral overall impact on total government spending. Some age-related programs, such as pensions and health care, will certainly witness an increase in spending due to aging, but others, such as education, workers’ compensation and justice, will benefit from a decrease in spending due to the aging of the population. Overall, the government will have the ability to offset increases in one area with decreases in others and there might be no need to smooth tax rates at all.
In point 2 above I take society’s perspective. However, society does not comprise the same individuals in all years, and those who make the contributions are usually younger than those who reap the benefits of prescription drug coverage. As a result, even in the absence of any compelling case for smoothing in terms of cost-efficiency from society’s perspective, there might still be a case for smoothing as a way to make generations accountable for their consumption of prescription drugs instead of letting them rely on the next generations. This is a fairness argument. The younger generation cannot be held responsible for the fact that they are less numerous than their parents’ generation (due to the low fertility rates of the latter) and therefore should not be asked to pay for the spending of their parents.
This is a tricky argument, almost of the “slippery slope” type. After all, if we truly want to make generations accountable for their fertility level, a within-generation issue immediately arises. The high-fertility individuals (say, two or more children) might be tempted to tax the low-fertility ones (one child or no children), who are truly responsible for the intergenerational imbalance. One would then have to calculate a fair compensation from the have-nots (no children) to the haves (children), but would need to take into account all the transfers, such as free education, already flowing from childless to child-rich households in Canada. This in turn suggests that the intergenerational-fairness issue based on the respective sizes of parent and child cohorts is somewhat exaggerated. After all, baby boomers had fewer children but also had children with a much higher level of human capital per capita. This investment in human capital came at a cost and made the current generation richer and, as a result, in a better position to pay for the prescription drugs of their parents.
The above argument suggests that per capita spending and contribution are not the end of the story in terms of intergenerational fairness. In fact, this is true of almost all public programs. But another investment-related feature of pharmacare makes the intergenerational-fairness argument even less compelling. It is true that when we spend on prescription drugs today, the sick (hence old) benefit more than the healthy (hence young). However, let us not forget that any expenditure on health care goes into the pocket of a health care provider; this is the fundamental equation of health economics (Evans 1984). In the case at hand, the health care provider is a pharmaceutical company that will invest at least some of the income thus generated in research and development. Pharmaceutical R&D will in turn generate prescription drug spending by future generations – that is, those who contribute today. The good news for these future generations is that at least some of their drug consumption will translate into longer and better lives for themselves.3 Thus the children of baby boomers are not only helping their low-fertility parents to purchase their prescription drugs (which is potentially unfair) but helping to secure more years of good health in their own old age.
If the benefit of longer life for the contributing generation exceeds the cost of supporting a large parental generation, there might not be a fairness issue after all. It all boils down to one critical issue: How many future quality-adjusted life years (or any other measure of quality of health care) do we buy with dollars spent on prescription drugs? And, more fundamentally, do we want to buy that or other goods and services (e.g., education, welfare transfers, housing benefits)?
Let me try a back-of-the-envelope estimate. If the next generation lives an average of five years longer than the parental one, and if one year of life is valued at a conservative $50,000, the total benefit for that generation will be $250,000 over the life course. This amounts to approximately $3,000 per year of life (assuming a life expectancy of 80 years). Now, following Cutler (2004), we can attribute to health care half of that increase in life expectancy; since pharmacare buys 10 percent of health care, we can attribute 5 percent of these $3,000 per year of life, or $150 per year of life to pharmacare. The benefit for the current generation of spending on prescription drugs seems larger than the cost of not smoothing (which would amount to $140 per year between now and 2050). As a result, even younger cohorts will benefit from the financing of R&D today, through their support of their parents’ consumption of prescription drugs.
Overall, I do not believe that prefunding pharmacare will enhance well-being or fairness. Recommendations for prefunding are based on premises that, as I have argued above, are not supportable.
To summarize, these premises are that prescription drug utilization is similar to age-related consumption and that population aging will be a substantial driver of that consumption at the aggregate level. I do not think that population aging will have such a dramatic effect on total spending on prescription drugs, but, more importantly, I think that the main driver of spending on prescription drugs will be (as it is now) medical progress, the fact that innovative and effective drugs are produced and used to generate longer, healthier lives. As a result, there is no doubt that more money, and very likely a greater share of national income, will go into prescription drugs in 2050 than is the case now.
This will certainly generate complex issues of distributive justice. If we collect revenues through (income-progressive) taxes, we make a large income transfer from the rich (who contribute more but benefit more or less equally) to the poor – a transfer that the middle class might very well object to. If we collect revenues based on flat-rate contributions (for example, through private insurance premiums), we generate inequality and potential inequity on the basis of ability to pay – the poor will not be able to access quality-of-life-enhancing drugs or will have to engage in catastrophic spending to do so.
One way of addressing such an issue is to base decisions about the public financing of prescription drugs on the benefit (in years of life and quality of life) generated by those drugs. Financing breakthroughs through the public purse and leaving “me toos” to the private insurance market would certainly help to contain the redistributive issue. It would not suppress the issue, though, because limiting ourselves to truly innovative drugs will still mean increased spending on prescription drugs in the future. Overall, this income-related issue is much more important and worrisome than the intergenerational-equity issue or the efficiency issue of separating the random from the systemic component of variability.
This publication was published as part of the the Faces of Aging research program under the direction of Sarah Fortin. The manuscript was copy-edited by Jane Broderick, proofreading was by Francesca Worrall and Freya Godard, editorial coordination was by Francesca Worrall, production was by Chantal Létourneau, art direction was by Schumacher Design and printing was by AGL Graphiques.
Jacqueline Greenblatt graduated with a master’s in public policy from the University of Toronto’s School of Public Policy and Governance in 2009. She currently works for the government of Canada in the field of evaluation and performance measurement.
Michel Grignon is an associate professor in the Department of Economics and the Department of Health, Aging and Society, and the associate director of the Centre for Health Economics and Policy Analysis at McMaster University. He is also an associate member of Institut de Recherche en Économie de la Santé in Paris, France.
Mark Stabile is director of the School of Public Policy and Governance at the University of Toronto and associate professor of economics at the Rotman School of Management. He is also a research Associate at National Bureau of Economic Research, Cambridge, Massachusetts, and a fellow at the Rimini Centre for Economic Analysis, Italy.
To cite this document:
Stabile, Mark and Jacqueline Greenblatt. 2010. “Providing Pharmacare for an Aging Population: Is Prefunding the Solution?” With a commentary by Michel Grignon. IRPP Study, No. 2.

